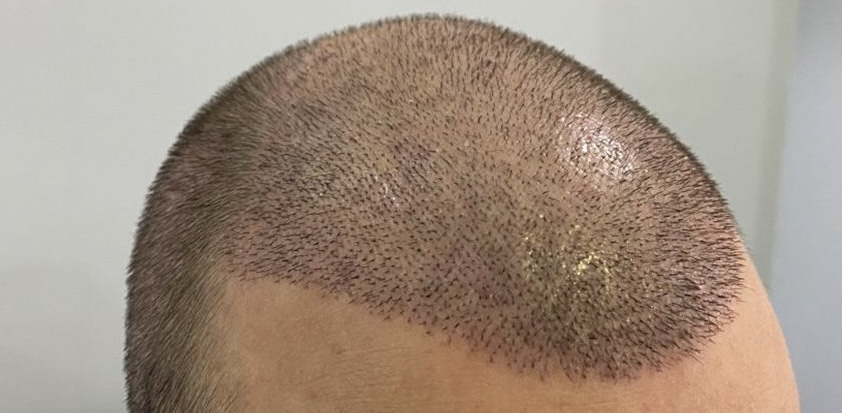
You’ve had your hair transplant. The procedure went well. The clinic was pleased with how it looked immediately after. And then, somewhere between week three and month four, you look in the mirror and the result seems thinner than you expected — possibly thinner than it looked before you had anything done at all.
This experience is so common that it deserves its own dedicated explanation, because the gap between what patients expect to see in the first months and what they actually see is one of the primary sources of post-procedure anxiety, regret, and unnecessary panic. The thinness you’re seeing in the first months is not a sign that something went wrong. It is not evidence of poor graft survival. It is not the final result.
It is biology doing exactly what it’s supposed to do — on a timeline that most patients weren’t adequately prepared for.
This guide explains the complete biological picture behind why hair transplant density looks thin in the first months: what’s happening at each stage, why the hair appears sparse even when the procedure was successful, what factors influence how thin the early months look, and how to read the signs that genuine progress is happening even when you can’t see it yet.
The Fundamental Misunderstanding About Hair Transplant Timelines
The most common expectation patients carry into the early recovery period is that the procedure will produce visible improvement on a timeline measured in weeks rather than months. Before-and-after galleries show dramatic transformations. Consultation materials describe the result at twelve months. But the psychological anticipation of seeing something — anything — tends to operate on a much shorter timeline than the biology actually allows.
This mismatch between anticipated and actual timeline is the root cause of most post-procedure distress about density. Understanding the actual biological sequence — not just knowing intellectually that it takes time, but understanding precisely why each phase looks the way it does and what’s happening underneath — is what transforms the waiting period from an anxious ordeal into a comprehensible process.
The reality is that a hair transplant doesn’t produce its result at the time of the procedure. The procedure creates the biological opportunity for a result. The result itself is produced by a series of biological processes — healing, follicle cycling, revascularization, anagen re-entry — that unfold over twelve to eighteen months after the procedure is complete. Every stage of that process has its own visual appearance, and the early stages look thin by design rather than by failure.
Stage One: The First Two Weeks — Apparent Density That Doesn’t Last
In the immediate days after a hair transplant, the transplanted area can look surprisingly full. The grafts are implanted with their existing hair shafts intact, and in the days before any shedding begins, the recipient area contains both the transplanted hairs and whatever native hair remained in the zone before the procedure.
This immediate post-procedure density is genuinely present but misleading as a predictor of the eventual result. The transplanted hair shafts you can see immediately after the procedure are not the permanent hair that will grow from these follicles long-term. They are the hairs the follicles were producing at the time of extraction — existing shafts that will shed as part of the normal biological response to the transplant process.
Patients who feel encouraged by what the area looks like in the first week or two are setting themselves up for a difficult transition when shedding begins, because that early density is temporary. The grafts are in the process of integrating into their new tissue environment, and the hairs they arrived with are about to follow a biological course that looks like loss before it looks like growth.
Stage Two: Shock Loss — Why the Area Looks Worse Than Before the Procedure
Between weeks two and eight for most patients — though the timing varies — the transplanted area enters what is clinically called shock loss, or telogen effluvium. The transplanted follicles, having experienced the cumulative stress of extraction, handling, and implantation into new tissue, respond by entering telogen — the resting phase of the hair growth cycle — and shedding the hair shafts they were producing.
This is not graft loss. The follicles themselves are alive and present in the scalp. What’s happening is a synchronized reset of the follicle’s growth cycle: the hair shaft is shed, the follicle enters a resting phase, and then — eventually — it will re-enter anagen and begin producing a new, permanent hair shaft from its new location.
But during the shedding phase, the visual experience is disconcerting. Hair that was there is gone. The recipient area may look sparser than it did before the procedure. Patients who were expecting to see improvement find themselves looking at a scalp that appears to have gotten worse.
Shock loss can also affect native hair in the recipient zone — hair that wasn’t transplanted but was present in or near the area where the procedure was performed. The tissue disruption of creating recipient channels, the inflammatory response of the healing process, and the general physiological stress of the procedure can push neighboring native follicles into telogen along with the transplanted ones. This native hair shock loss is temporary and will also recover, but it adds to the apparent thinness of the early months.
Understanding that shock loss is a cycle reset rather than a failure is critical for navigating this phase emotionally. The follicles that shed their hairs during this phase are not departing — they are resting, underground, preparing for the growth phase that will produce the actual permanent result.
Stage Three: The Waiting Period — Months Two Through Four
After the shedding phase, most patients enter what is genuinely the most psychologically difficult stretch of the entire hair transplant timeline: a period of two to three months where essentially nothing visible is happening.
The follicles are in telogen. They are resting. They are not producing visible hair. The scalp may look thin or even bald in treated areas. There is no visible evidence of progress. Patients who don’t understand this phase interpret the absence of growth as evidence that growth is not coming — which is incorrect, but entirely understandable given what the mirror shows.
This phase is sometimes called the “ugly duckling” period of hair transplant recovery, and the name is apt. The scalp at month two or three looks nothing like what it will look like at month nine or twelve. The follicles are alive and preparing for their anagen re-entry, but that preparation is happening entirely underneath the surface of the scalp, with no visible indication of progress from above.
Several specific factors make this phase look particularly sparse:
The shock loss of native hair, if it occurred, has not yet reversed. The transplanted follicles are in telogen and not producing visible hair. The scalp surface in the recipient area, which has healed from the procedure, reflects light differently than scalp covered with hair — making it appear more exposed than it would in photographs taken under different lighting conditions. And the emotional anticipation of progress makes the absence of visible improvement feel more significant than it objectively is.
The practical implication of understanding this phase is simple: what you see in the mirror at months two and three has essentially no predictive value for what you will see at month nine. The two states are not on a continuum — they are separated by a complete biological cycle reset that hasn’t yet surfaced visually.
Why Revascularization Determines When Growth Begins
The timing of when transplanted follicles exit telogen and begin producing new hair is significantly determined by a process called revascularization — the growth of new blood vessels from the surrounding tissue toward the implanted follicles.
When a follicle is extracted from the donor area and implanted into the recipient site, it loses its established blood supply. In its new location, it must rely on nutrients from the surrounding tissue until new capillaries grow toward it and establish a direct blood supply. This revascularization process begins within the first days after implantation but takes weeks to establish adequately and months to fully mature.
Until revascularization has progressed sufficiently, the follicle remains in a quiescent, energy-conserving state. It is alive and metabolically active at a maintenance level, but it is not yet in a state where active hair production is supported by adequate blood flow. As revascularization matures and the follicle’s blood supply becomes more robust, the conditions for anagen re-entry are established.
This is one of the biological reasons why the crown area of the scalp — which has a somewhat less dense vascular network than the frontal scalp — tends to show new growth slightly later than the frontal zone in most patients. The revascularization timeline in the crown is slightly longer, which delays the anagen re-entry of transplanted follicles in that zone compared to those transplanted into the more vascularized frontal region.
It’s also one of the reasons why nutritional status matters during the recovery period. The development of new blood vessels is an energy and nutrient-intensive biological process. Patients who are iron-deficient, vitamin D-deficient, or who have inadequate protein intake are providing a less optimal biochemical environment for revascularization — which can contribute to slightly delayed or less robust early growth.
Stage Four: Early Growth — Months Three to Six
Somewhere between months three and five for most patients, the follicles begin exiting telogen and re-entering anagen. New hairs begin emerging from the scalp surface. This is the phase that patients have been waiting for — visible evidence that the procedure worked and that growth is underway.
But early growth looks nothing like the mature result, and this is another source of patient confusion during the recovery period. The first hairs to emerge from follicles returning from telogen are typically fine, light in color, and irregular in distribution across the recipient area. They may emerge in some zones before others. They may look wispy and sparse even when the underlying follicle density is adequate. The early growth phase looks thin not because the final density will be thin, but because the growth process is in its earliest stages.
The initial hair shafts produced by follicles returning from telogen are often finer than the mature hair these follicles will eventually produce. As the follicle completes its first full anagen cycle in its new location and establishes a more robust blood supply and tissue integration, subsequent hair cycles tend to produce progressively thicker, more pigmented shafts. The hair you see at month four is typically thinner in caliber than the hair you will see at month twelve, even if it’s emerging from the same follicle.
The distribution pattern of early growth also contributes to the sense of sparseness. Follicles don’t all exit telogen simultaneously — they come out in waves, with some areas showing growth while others are still in the resting phase. This irregular emergence pattern means that even when overall follicle survival was excellent, the early growth phase can look patchy and uneven in a way that doesn’t reflect the distribution of the eventual result.
Why Hair Caliber and Color Matter as Much as Count
One of the most underappreciated reasons why early hair transplant density looks thin even when graft survival was good is the relationship between hair caliber, pigmentation, and perceived density.
Visual density — how full the hair appears to the eye — is not simply a function of how many hairs per square centimeter are present. It is significantly influenced by the thickness of each individual hair shaft and the contrast between hair color and scalp color. Fine, light-colored hairs over a pale scalp create significantly less visual coverage per strand than coarse, dark hairs over the same scalp. The same number of follicles can look dramatically different depending on these characteristics.
In the early months of growth, transplanted hair tends to emerge thinner and sometimes lighter than it will eventually be. This means the visual density of the early result is doubly compromised: fewer hairs are present than will eventually be present, and the hairs that are present are finer than they will eventually be. Both factors work in the same direction — toward apparent sparseness that doesn’t reflect the eventual mature result.
As the hair matures through its first complete anagen cycle in the new location, both caliber and pigmentation tend to increase. Hair that looked thin and light at month four often looks noticeably thicker and darker at month nine, even without any change in the number of hairs present. This maturation of hair quality is one of the most important — and most overlooked — components of the improvement that continues through months six to eighteen.
The Role of Hair Length in Perceived Density
Another factor that makes early growth look thinner than it actually is relates to hair length. Short hair provides less coverage per strand than longer hair, because longer hair overlaps and layers in ways that create shadow and depth. When new growth first appears at month three to five, it is by definition short — emerging from the scalp at its absolute minimum length. As it grows longer through months five to nine, the same density of follicles produces progressively more visual coverage simply because longer hair provides more overlapping, layering, and shadow-creating coverage of the scalp beneath.
This means that the improvement patients see between months five and nine is driven by two overlapping processes: more follicles exiting telogen and producing new hairs, and the existing early-growth hairs becoming longer and providing more coverage per strand. The combination of these two effects is what produces the often dramatic-feeling improvement that most patients experience in the second half of the first year.
Patients who are evaluating their result at month four or five by looking at their hair very short — buzz-cut length or shorter — are seeing the worst possible representation of their result. The same follicle density looks dramatically different at two millimeters versus four centimeters of hair length, and evaluating density at the shortest possible length systematically underestimates what the result will look like when worn at any practical styling length.
How Lighting Conditions Distort the Perception of Density
The conditions under which patients evaluate their results significantly affect what they see — and the conditions that most patients use to evaluate their hair are systematically the worst possible conditions for assessing density accurately.
Overhead lighting, which is the most common indoor lighting in bathrooms, creates a downward angle of illumination that maximizes scalp visibility between hair shafts. Hair provides shading and coverage when light comes from the side or front, because it casts shadows that make the scalp beneath less visible. Under overhead lighting, that shading is eliminated — the light shines directly onto the scalp between hairs, making any gap in coverage maximally apparent.
This is true for everyone, not only for hair transplant patients. People with naturally dense hair look significantly thinner under overhead bathroom lighting than they do in outdoor natural light or under side-lit indoor conditions. But for patients who are anxiously monitoring their hair transplant result, the bathroom mirror under overhead lighting becomes the primary assessment condition — and it systematically makes the result look worse than it genuinely is.
Natural outdoor light, particularly diffused natural light that doesn’t cast harsh shadows, provides a significantly more accurate representation of actual hair density. The same scalp that looks concerningly thin in a bathroom mirror at month four often looks meaningfully better when assessed in outdoor conditions at the same timepoint. Patients who understand this lighting dynamic and actively seek out better assessment conditions during the recovery period navigate the waiting months with considerably less distress.
What Graft Survival Actually Looks Like
A common misunderstanding during the early months is conflating the apparent thinness of the early result with poor graft survival. Patients who see sparse early growth sometimes conclude that many grafts were lost — that the procedure didn’t take properly, or that something went wrong during recovery.
The reality is that graft survival cannot be meaningfully assessed before month six at the earliest, and a full assessment requires waiting until month twelve. The apparent thinness of months two through five reflects the biological cycle reset of shock loss and the early stage of anagen re-entry — not the absence of surviving follicles. A patient with excellent graft survival — ninety percent or higher — will go through exactly the same phase of apparent sparseness that a patient with lower survival goes through, because both are experiencing the same biological process.
The distinction between shock loss and graft loss only becomes visible with time. By month six, a meaningful picture begins to emerge: areas where follicles survived but are in early anagen show new growth; areas where follicles were not retained show no growth regardless of how long the patient waits. But in the months before this assessment is possible, the visual appearance of the recipient area tells patients very little about how their graft survival actually compared.
This is worth understanding clearly because the anxiety about graft survival in the early months is almost always premature and often inaccurate. The biological process of shock loss, telogen, and anagen re-entry is standard and expected. What looks like failure in month two or three is most often the normal biology of a successful procedure in progress.
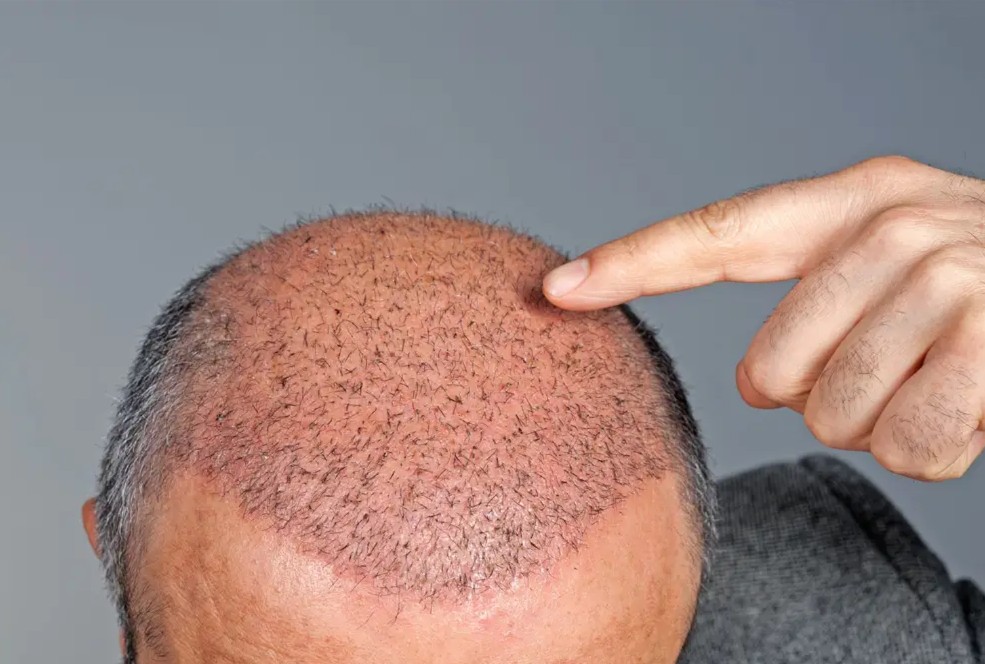
Factors That Influence How Thin the Early Months Look
While the early thinness is a universal feature of the recovery process, several factors influence how pronounced it looks for any individual patient.
Hair characteristics — particularly caliber, color, and curl — have a significant effect on how much coverage even sparse early growth provides. Patients with naturally coarse, dark, wavy hair will notice their early growth providing more visual coverage per strand than patients with fine, light, straight hair. The latter group tends to experience the early months as looking thinner, even when follicle survival and anagen re-entry are progressing identically.
The extent of native hair loss at the time of the procedure affects how dramatic the early months look. A patient who had some remaining native hair in the recipient zone benefits from that hair continuing to provide coverage even during the period when transplanted follicles are in shock loss. A patient with more complete baldness in the recipient zone has no native hair buffer — the shock loss of transplanted follicles leaves a scalp with no coverage at all, making the early months visually more dramatic.
The density of the procedure influences how early growth looks. High-density procedures, while ultimately producing better results, go through a shock loss phase where more follicles are simultaneously in telogen — which can make the apparent density during that phase look particularly low. Lower-density procedures have fewer follicles simultaneously in shock loss, which can make the early months look somewhat less sparse even though the long-term result will be less dense.
Nutritional status influences the pace of revascularization and anagen re-entry. Patients who are iron-deficient, particularly those with low ferritin, tend to experience more pronounced and prolonged telogen and slower anagen re-entry than nutritionally replete patients. Ensuring adequate ferritin, vitamin D, zinc, and protein intake during the recovery period supports the biological conditions for earlier and more robust growth emergence.
Medical management of ongoing hair loss with finasteride or minoxidil affects how much native hair is preserved during and after the recovery period. Patients using finasteride maintain more of their existing native hair through the recovery period, which provides more coverage during the months when transplanted follicles are in shock loss. Patients without medical management may find that native hair thinning progresses during the recovery period, compounding the appearance of sparseness.
The Crown: Why It Takes Even Longer
Patients who have crown transplants face an extended version of the early thinness experience, because the crown consistently shows new growth later than the frontal zone and takes longer to reach its full mature density.
The reasons are anatomical. The crown has a somewhat less dense vascular network than the frontal scalp, which means revascularization of implanted grafts proceeds more slowly. The spiral growth pattern of the crown means that early growth hairs radiate outward in multiple directions, with each hair providing less unidirectional coverage per unit of length than frontal hairs all growing in the same forward direction. Crown hairs take longer to reach the length at which their overlapping coverage creates the visual density effect that makes hair look full.
Crown results are frequently substantially incomplete at nine months, continue developing through twelve months, and in many patients reach their full maturity somewhere between twelve and eighteen months. Patients evaluating a crown result at six months and feeling disappointed should understand that they are seeing an early chapter of a story whose conclusion hasn’t been written yet.
Month Six Through Twelve: When Density Becomes Visible
For most patients, the experience of seeing density accumulate rather than simply looking thin begins somewhere between months five and seven. This is the phase where the combination of more follicles exiting telogen, longer hair providing more coverage, and maturing hair caliber creates the experience of visible improvement.
The improvement often feels non-linear — periods of apparent stasis followed by noticeable jumps — because it reflects the wave-like pattern of follicle anagen re-entry and the compounding effect of multiple factors improving simultaneously. Patients in this phase often describe a moment of recognition — looking in the mirror and seeing for the first time that the result is actually working, that there is genuinely more hair than there was, that the density is building toward something real.
By month nine to twelve, most patients have a substantially complete picture of their result, though refinement continues. The density present at twelve months typically reflects eighty to ninety percent of the mature final result, with some continued improvement through month eighteen from follicles that entered anagen later and from continued maturation of hair caliber in follicles whose first anagen cycles produced finer initial shafts.
How to Navigate the Early Months
Knowing that the thinness of the early months is expected, biological, and temporary doesn’t make it emotionally easy — but it makes it manageable in a way that genuine uncertainty wouldn’t.
The most practical approach to the early months is to establish assessment conditions that aren’t systematically biased toward looking thin. Assess hair under natural outdoor light rather than overhead bathroom lighting. Assess at the hair length you actually wear rather than at the shortest possible length. Take photographs at consistent intervals under consistent conditions to track genuine progress rather than relying on daily mirror assessments that capture random variation in lighting and styling rather than biological change.
Understand the timeline specifically rather than vaguely. Not “it takes time” but “follicles are in telogen until months three to five, early anagen produces fine short hairs through months five to seven, caliber and length mature through months seven to twelve, full assessment requires twelve months.” Having the specific biological sequence in mind allows you to locate yourself accurately in the process rather than floating in undefined waiting.
At Hairpol, post-procedure support includes specific communication about what to expect at each phase of the recovery timeline — not because the thinness of the early months can be prevented, but because patients who understand what they’re seeing navigate the process with significantly more confidence than those who encounter it without preparation.
The density will come. The biology is working. The thin months are not the result — they are the path to the result, doing exactly what it is designed to do.
Frequently Asked Questions (FAQ)
Why does my hair look thin after a hair transplant?
The thinness you see in the first months after a hair transplant is a normal and expected part of the biological recovery process — not a sign that something went wrong. Transplanted follicles respond to the stress of extraction and implantation by entering telogen, the resting phase of the hair growth cycle, and shedding the hair shafts they were producing. This is called shock loss. During and after shock loss, the recipient area can look sparse or even thinner than before the procedure. The follicles themselves are alive and present in the scalp — they are resting, not lost. The thinness of the early months reflects the biological cycle reset in progress, not the quality or outcome of the procedure.
When does hair start growing after a hair transplant?
New hair growth from transplanted follicles typically begins appearing between months three and five after a hair transplant, as follicles exit telogen and re-enter anagen — the active growth phase. However, this early growth looks nothing like the mature result. The first hairs to emerge are typically fine, light in color, and unevenly distributed across the recipient area. Visual density accumulates progressively through months five to nine as more follicles exit telogen, existing hairs grow longer and provide more overlapping coverage, and hair caliber matures. A substantially complete picture of the result is typically visible by months nine to twelve, with continued refinement through month eighteen on the hair transplant timeline.
Is shock loss after a hair transplant permanent?
No — shock loss after a hair transplant is temporary, not permanent. Shock loss, or telogen effluvium, occurs when transplanted follicles enter the resting phase of the hair growth cycle in response to the stress of the procedure. The follicles shed their existing hair shafts but remain alive in the scalp. They will exit telogen and re-enter the active growth phase, typically beginning to produce new hair between months three and five. Native hair in the recipient zone that experienced shock loss from the tissue disruption of the procedure also recovers on a similar timeline. The apparent thinness of shock loss is a temporary phase in a biological cycle reset — the follicles that shed during this phase are working their way back to growth, not departing permanently.
Why does my hair transplant look worse at month two than at month one?
Looking worse at month two than month one after a hair transplant is one of the most common — and most distressing — experiences of the recovery period, and it is entirely normal. In the first days after the procedure, the transplanted area contains both the newly implanted grafts and their existing hair shafts, which can create an impression of reasonable density. As shock loss progresses through weeks two to eight, those hair shafts shed and the recipient area enters its most sparse phase. Additionally, shock loss can affect native hair in and around the recipient zone, compounding the apparent thinness. Month two often represents the lowest visual point of the entire recovery process. By months three to five, follicles begin exiting telogen and new growth starts to emerge — the biological process is moving in the right direction even when the mirror suggests otherwise.
How long does the thin phase last after a hair transplant?
The thin phase after a hair transplant typically lasts from approximately weeks two through month four or five for most patients, though individual timing varies. The shedding phase of shock loss runs from roughly weeks two to eight. After shedding concludes, follicles remain in telogen — the resting phase — for an additional two to three months, producing no visible hair. New growth begins emerging around months three to five, initially as fine, sparse hairs that gradually thicken and multiply. The experience of visible density accumulating — the end of the thin phase — typically begins somewhere between months five and seven. For crown transplants, the thin phase can extend somewhat longer, with meaningful density often not appearing until months six to eight given the crown's longer revascularization timeline.
Does bathroom lighting make a hair transplant look thinner than it really is?
Yes — overhead bathroom lighting is one of the worst possible conditions for accurately assessing hair transplant density, and systematically makes the result look thinner than it genuinely is. Overhead lighting shines directly downward onto the scalp, maximizing scalp visibility between hair shafts and eliminating the side-cast shadow that makes hair look fuller under other lighting conditions. This effect applies to everyone — people with naturally dense hair look significantly thinner under overhead bathroom lighting than in natural outdoor light. For patients anxiously monitoring their recovery, assessing the result primarily in bathroom mirror conditions leads to consistent underestimation of actual density. Natural outdoor diffused light provides a significantly more accurate representation. Taking progress photographs outdoors under consistent lighting conditions gives a much more reliable picture of how the result is actually developing through the hair transplant timeline.
Why does early hair transplant growth look fine and sparse even when graft survival was good?
Early growth after a hair transplant looks fine and sparse even with good graft survival for two overlapping reasons. First, the initial hair shafts produced by follicles returning from telogen are typically finer and sometimes lighter in color than the mature hair these follicles will eventually produce. As follicles complete their first full anagen cycle in their new location and establish more robust blood supply and tissue integration, subsequent hair cycles produce progressively thicker, more pigmented shafts. Second, early growth hairs are by definition short — and short hair provides significantly less coverage than longer hair that overlaps and layers to create shadow and depth. The combination of fine caliber and short length means that even good follicle density looks sparse at month four. Both factors improve progressively through months five to twelve as hair matures in caliber and grows in length.
When can I accurately assess my hair transplant result?
A meaningful assessment of a hair transplant result requires waiting until at least month nine, and a fully accurate assessment requires month twelve. Before month nine, the result is still developing — follicles may still be exiting telogen and entering anagen, hair caliber is still maturing, and hair length is still increasing. Any assessment before this point captures an incomplete picture of a process in progress rather than the actual result. The distinction between areas of shock loss recovery and areas of genuine lower graft survival cannot be reliably made before month six. Crown transplants require evaluation at twelve to eighteen months rather than nine to twelve, given the crown's longer revascularization timeline and later growth emergence. Assessing results under natural outdoor light rather than overhead bathroom lighting, and at the hair length you actually wear rather than the shortest possible length, produces a significantly more accurate picture of the genuine outcome.