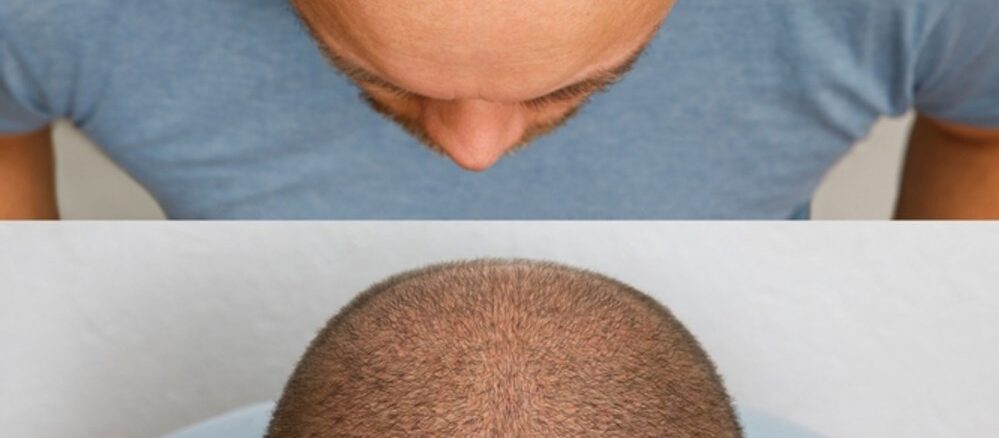
Nobody warns you clearly enough. You go through the procedure, you get through the first week of careful washing and elevated sleeping and avoiding the gym, and then — somewhere between week two and week eight — the hair starts falling out.
Not thinning. Falling out. Visibly. In the shower, on the pillow, in your hands when you accidentally touch the scalp too firmly.
The natural reaction is panic. The natural thought is that the transplant failed, that the grafts didn’t take, that the money and the trust and the recovery time were wasted. Patients search frantically online at 2am looking for reassurance or confirmation of their worst fears, and they find both — which makes everything worse.
Here is the honest, complete explanation of what’s actually happening, why it happens to almost everyone, and what it means for your final hair transplant results.
The Short Answer First
The hair falls out. The follicles don’t.
That distinction is everything. When transplanted hair sheds in the weeks after a hair transplant, the visible shaft — the part you can see above the scalp — detaches and falls. But the follicle, the living root structure implanted beneath the skin, stays exactly where it was placed.
The follicle enters a resting phase. It goes quiet. And then, on its own timeline, it wakes up and begins producing new hair from scratch.
This is not failure. This is how transplanted hair works. The shedding is not a warning sign. It is a biological step in a process that eventually produces permanent, growing hair.
What Actually Happens to a Hair Follicle During Transplantation
To understand why shedding happens, it helps to understand what a follicle experiences during the procedure.
During a hair transplant — whether Sapphire FUE, DHI, or another technique — individual follicular units are extracted from the donor area, usually the back and sides of the scalp where hair is genetically resistant to loss. These follicles are then carefully implanted into the recipient zone: the areas experiencing thinning or baldness.
The moment a follicle is extracted, it is separated from its blood supply. It’s kept in a preservation solution, handled with precision instruments, and implanted within a specific window of time to preserve viability. But no matter how careful the process, the follicle has been through a significant physical event.
Once implanted, the follicle begins reconnecting to its new environment. New blood vessels grow toward it. The surrounding tissue starts integrating around it. This process — called revascularization — takes time, and in the meantime, the follicle is operating under stress.
The hair shaft attached to that follicle responds to this stress by entering what’s called the telogen phase, or resting phase. It releases the visible hair and shuts down active growth temporarily while the follicle stabilizes, reconnects, and recovers.
This is not damage. This is a protective response.
The Hair Growth Cycle and Why It Explains Everything
Hair doesn’t grow continuously. It grows in cycles, and every follicle on your scalp is at a different point in that cycle at any given time.
The three main phases are:
Anagen — the active growth phase. This is when the follicle is producing the hair shaft and pushing it upward. Anagen lasts anywhere from two to six years depending on genetics, and this is why some people can grow very long hair and others can’t.
Catagen — a short transitional phase lasting a few weeks where growth slows and the follicle prepares to rest.
Telogen — the resting phase, lasting roughly two to four months. The hair shaft is retained but not actively growing. At the end of telogen, the old shaft is released and a new anagen cycle begins, pushing fresh hair upward from the same follicle.
When a follicle is transplanted, the trauma of extraction and implantation forces it prematurely into telogen — regardless of where it was in its natural cycle. The follicle essentially says: conditions have changed dramatically, I need to pause, reset, and stabilize before I continue.
The visible hair falls out. The follicle rests. Then it restarts.
This is why transplanted hair falls out before it grows back — because the follicle’s growth cycle has been interrupted and reset, not because the follicle itself has been lost.
When Does the Shedding Start and How Long Does It Last?
The shedding phase — often called shock loss in the context of hair transplant recovery — typically begins somewhere between two and six weeks after the procedure. For some patients it starts closer to week two. For others it doesn’t become noticeable until week five or six.
The variation is normal and doesn’t indicate anything about the quality of the result. It reflects individual differences in follicle response, the proportion of grafts that were already in or near telogen at the time of transplant, and general scalp characteristics.
The shedding itself usually plays out over two to four weeks. It rarely happens all at once — more often it’s a gradual process where you notice more hair on the pillow than before, or more loss during washing, or simply look at the transplanted area and realize it looks thinner than it did in week two.
By months two to three, the shedding has typically finished. The scalp enters what many patients describe as the quietest and most difficult phase of the hair transplant timeline — a period where very little seems to be happening on the surface while the follicles are in various stages of their resting and restarting cycles underground.

What Shock Loss Looks Like in Practice
Shock loss doesn’t look the same for everyone, and the variation can cause unnecessary anxiety when patients compare their experience to someone else’s.
Some patients shed the majority of transplanted hairs within a few weeks and are left with a scalp that looks almost identical to — or temporarily worse than — how it looked before the procedure. This is the scenario that most often triggers the fear that something has gone wrong.
Other patients experience more gradual shedding and retain some of the transplanted hair during the resting phase. These patients often feel more psychologically comfortable during months two and three, even though their long-term result will be similar to the first group.
The amount of shedding doesn’t predict the final outcome. Two patients with identical graft counts and identical techniques can have very different shedding patterns and arrive at similar results by month twelve.
Native hair — the non-transplanted hair in and around the recipient area — can also experience temporary shock loss in response to the trauma of the surrounding procedure. This is more common when transplantation has been performed near existing hair and usually resolves as the scalp heals. It can make the overall appearance look thinner than expected in the early months, which compounds the psychological difficulty of this phase.
Why the Follicle Survives Even When the Hair Doesn’t
This is the part that most patients find hardest to believe when they’re watching hair fall out in the shower.
The follicle and the hair shaft are not the same thing. The shaft — the visible strand — is essentially a non-living structure produced by the follicle. It’s made of keratinized cells, meaning it has no blood supply of its own and no biological function beyond the cosmetic and the protective.
When the shaft falls out during the shedding phase, it’s releasing something that was going to fall out anyway at the end of its natural telogen cycle. The follicle itself — the living, blood-supplied structure below the skin — remains in place.
Provided the grafts were properly placed and survived the initial implantation window, the follicle will eventually restart its growth cycle. The anagen phase returns. A new hair shaft is produced. It pushes upward through the skin, typically beginning to appear somewhere between months three and five after the procedure.
This is why the hair transplant timeline consistently places visible regrowth in the three to six month range rather than the first few weeks. The follicles need the resting phase to stabilize before they can sustain active growth again.
The Emotional Reality of the Shedding Phase
It’s worth being direct about this: the shedding phase is psychologically hard for most patients, and the difficulty is often underestimated before the procedure.
You’ve made a significant decision. You’ve gone through a surgical procedure. You’ve followed every instruction carefully. And now, weeks later, you look worse than you did before you started.
That experience produces genuine distress for many people. It’s not irrational. It’s a completely understandable response to a visible change that appears to contradict the expected direction of progress.
What helps is understanding clearly — before the shedding begins — that this phase is not evidence of failure. It is a predictable, documented, nearly universal part of how hair transplants work. Clinics that explain the timeline honestly will tell you this before your procedure. If you weren’t told, it doesn’t mean something unusual is happening. It means you needed more information.
The patients who handle the shedding phase most calmly are almost always the ones who were told clearly what to expect and when. The anxiety lives in the gap between expectation and reality. Close that gap with information, and the phase becomes something you move through rather than something that moves you.
What Regrowth Actually Looks Like
When the follicles begin their new anagen cycle, the first hairs to emerge are often different from what patients expect.
Early regrowth hair is typically:
- Fine and soft, almost like vellus hair
- Slightly lighter in color than the final hair will be
- Sometimes slightly wavy or irregular in texture
- Thin enough that it adds little visible coverage in the early weeks
This is normal. The shaft produced in the first new growth cycle after transplantation is rarely the final, mature version of the hair. It takes time for the follicle to settle into its new environment and begin producing hair with its full natural characteristics.
Between months four and six, the hair becomes progressively more visible. Coverage starts to look real rather than sparse. By months six through nine, most patients are in the phase where they notice consistent improvement and begin to feel confident about the direction of their result.
Months nine through twelve — and in some cases extending to eighteen months for certain areas like the crown — represent full maturation. The hair has thickened, darkened, and behaved more naturally. This is when the result of a successful hair transplant becomes what it’s going to be long-term.
How to Tell If Something Is Actually Wrong
The shedding phase is normal. But it shouldn’t be used as a blanket reassurance that masks genuine problems.
There are situations where hair loss after a hair transplant indicates something other than the expected cycle reset.
Contact your clinic and seek a follow-up assessment if:
- Shedding continues beyond month three with no signs of any new growth beginning
- You develop persistent scalp pain, heat, or discharge that suggests infection
- Certain areas show absolutely no regrowth while others have started growing normally — this can sometimes indicate graft survival issues in specific zones
- You had a procedure and were not informed of the shedding phase at all, and your clinic is now unreachable or dismissive when you raise concerns
For the vast majority of patients at reputable clinics, none of these apply. The timeline progresses as expected, new growth begins in months three to five, and the result develops steadily from there.
But genuine concerns deserve genuine answers. If something feels medically wrong — not just emotionally uncomfortable — pursue a proper clinical conversation rather than relying entirely on forum reassurance.
The One Thing to Remember
Every question about the shedding phase comes back to the same biological reality: the hair is not the follicle.
When transplanted hair falls out in the weeks after your procedure, you are not losing your grafts. You are watching the hair shaft complete its interrupted cycle while the follicle rests and resets beneath the surface.
The follicle is there. It is alive. It is going to grow again.
That process takes months, not weeks. The hair transplant timeline is measured in seasons, not days. Patients who understand this — who can hold onto the biological reality rather than the emotional response to a mirror — move through the shedding phase with significantly less distress and arrive at the growth phase with their expectations calibrated correctly.
The hair fell out. That part of the story isn’t finished. It’s just at the pause before the next chapter.
Frequently Asked Questions (FAQ)
Is it normal for transplanted hair to fall out after a hair transplant?
Yes, it is completely normal for transplanted hair to fall out in the weeks following a hair transplant. This process is known as the shedding phase or shock loss, and it occurs in nearly every patient. The visible hair shaft detaches and falls while the follicle — the living root structure beneath the skin — remains intact and in place. The follicle enters a temporary resting phase before restarting its growth cycle and producing new hair. Shedding during this phase is not a sign of graft failure. It is a predictable biological response to the stress of extraction and implantation.
When does the shedding phase start after a hair transplant?
The shedding phase after a hair transplant typically begins between two and six weeks following the procedure. For some patients the shedding becomes noticeable as early as week two, while for others it doesn't appear until week five or six. The variation in timing is normal and does not indicate anything about the quality of the result or graft survival. The shedding usually plays out gradually over two to four weeks rather than all at once, and by months two to three the active shedding phase has typically concluded for most patients. What follows is a quieter waiting period before new regrowth begins to emerge.
Will my hair grow back after the shedding phase?
Yes. The follicles that shed their visible hair shafts during the shedding phase remain alive beneath the scalp and will restart their growth cycle. The hair shaft and the follicle are not the same structure — the shaft is a non-living product of the follicle, and its loss during shedding does not mean the follicle has been lost. Provided the grafts were properly placed and survived the initial implantation window, new hair will begin emerging from the follicles as they re-enter the anagen growth phase. Visible regrowth typically begins appearing between months three and five on the hair transplant timeline, with density continuing to develop through months six to twelve.
What is the difference between shock loss and normal shedding after a hair transplant?
In the context of hair transplant recovery, shock loss and the shedding phase refer to the same phenomenon — the stress-induced loss of transplanted hair as follicles enter a temporary telogen phase. However, shock loss can also affect native hair — the existing non-transplanted hair in and around the recipient area — which sheds temporarily in response to the trauma of the procedure happening around it. Native hair shock loss tends to begin slightly later than transplanted hair shedding and is more common when transplantation was performed near areas with existing hair. Both types are temporary and the follicles involved will produce new hair as the growth cycle restarts.
How long does it take for transplanted hair to grow back after shedding?
After the shedding phase concludes, the follicles enter a resting period before restarting active growth. Visible new hair from transplanted follicles typically begins appearing between months three and five following the procedure. This early regrowth is often fine, soft, and lighter in color than the final mature hair — this is normal and reflects the follicle's initial growth cycle in its new environment. Between months four and six coverage becomes progressively more visible, and by months six through nine most patients notice consistent density improvement. Full maturation — where the transplanted hair has thickened to its permanent characteristics — typically occurs between months nine and twelve, with crown areas sometimes continuing to develop through month eighteen on the hair transplant timeline.
Does heavy shedding mean my hair transplant failed?
No. The amount of shedding during the shedding phase does not predict the final outcome of a hair transplant. Two patients with identical graft counts and identical techniques can experience very different shedding patterns — one dramatic and rapid, one gradual and mild — and arrive at comparable results by month twelve. Heavy shedding that leaves the scalp looking similar to or temporarily worse than it did before the procedure is an emotionally difficult experience but is not evidence of graft loss. The distinction between shock loss — where follicles are resting and will regrow — and actual graft loss only becomes clear over time, as regrowth beginning between months three and five confirms that the follicles survived.
Can native hair also fall out after a hair transplant?
Yes, native hair — the existing non-transplanted hair in and around the recipient area — can experience temporary shock loss following a hair transplant. This occurs when the follicles of existing hair are disturbed by the tissue trauma of the procedure happening around them — the creation of recipient channels, the handling of the scalp during implantation, and the general inflammatory response. Native hair shock loss tends to begin slightly later than transplanted hair shedding, often becoming apparent around weeks three to six. It is more common when transplantation was performed near areas with significant existing hair. The affected follicles remain alive and will produce new hair as the growth cycle restarts, typically in the same three to five month timeframe as transplanted hair regrowth.
When should I be concerned that my shedding is not normal?
The shedding phase after a hair transplant is normal in the vast majority of cases and resolves without clinical intervention. However, there are specific circumstances that warrant contacting your clinic for a proper assessment. These include shedding that continues beyond month three with no signs of any new regrowth beginning, persistent scalp pain, heat, or discharge suggesting infection, specific zones showing no regrowth at all by month five or six while neighboring areas have clearly started growing, or any situation where a clinic is unreachable or dismissive when legitimate concerns are raised. The emotional discomfort of the shedding phase is expected and normal. Symptoms that suggest a medical issue rather than a psychological one — ongoing pain, discharge, or complete absence of growth well past the expected hair transplant timeline — deserve professional evaluation.