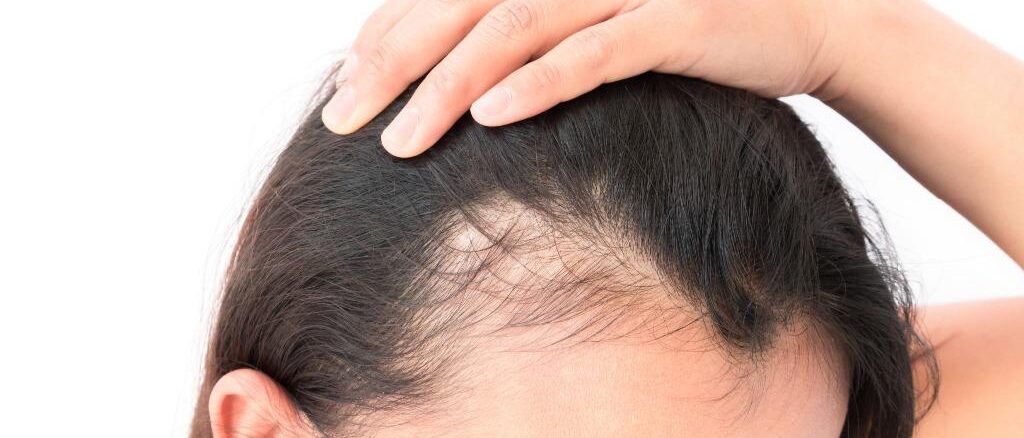
Stress is one of the variables in hair transplant recovery that receives the least specific attention in post-procedure guidance — and one of the most consequential. Patients are told to rest, avoid strenuous activity, and follow their aftercare protocol carefully. They are rarely told in specific terms how psychological and physiological stress affects the biological processes that determine how well their grafts survive, how quickly they recover from shock loss, and how robustly new growth emerges in the months that follow.
This is a meaningful gap in most aftercare guidance. Stress influences hair loss biology in ways that are well-documented in the clinical literature, and the specific mechanisms through which it does so are directly relevant to the post-transplant recovery period. Understanding how stress interacts with the biological processes of graft survival and hair growth — and what practical steps can moderate its impact — gives patients a more complete picture of what recovery actually involves and a more realistic framework for managing it.
This guide covers the complete picture: the biology of how stress affects hair follicles, how those mechanisms interact specifically with hair transplant recovery, the specific types of stress most relevant to the post-procedure period, and practical strategies for managing stress in ways that support rather than undermine the result being grown.
The Biology of Stress and Hair Loss
The relationship between stress and hair loss is not folk wisdom — it is a well-characterized biological phenomenon with specific mechanisms that operate at the follicle level. Understanding these mechanisms is the foundation for understanding why stress management matters specifically in the post-transplant context.
The primary pathway through which psychological stress affects hair follicles involves the hypothalamic-pituitary-adrenal axis — the hormonal cascade that the body activates in response to perceived threats. When the brain perceives a stressor, the hypothalamus signals the pituitary gland, which signals the adrenal glands to release cortisol — the body’s primary stress hormone. Sustained cortisol elevation, as occurs in chronic rather than acute stress, has specific and documented effects on hair follicle biology.
Elevated cortisol promotes the entry of hair follicles into the telogen phase — the resting phase of the hair growth cycle — through several mechanisms. Cortisol inhibits the activity of growth factors that support the anagen phase, including insulin-like growth factor-1 (IGF-1) and fibroblast growth factor (FGF), both of which promote follicle cycling into active growth. It also stimulates the production of substance P, a neuropeptide that has been shown to promote premature telogen entry in follicles. The result is a stress-induced shift in the hair growth cycle toward telogen — which produces the clinical pattern called telogen effluvium: diffuse shedding that typically begins two to three months after a significant stressor, reflecting the delayed telogen entry and shedding that characterizes the follicle’s stress response.
Cortisol also affects scalp blood flow by promoting vasoconstriction — narrowing of blood vessels that reduces circulation to peripheral tissue including the scalp. In the post-transplant context, where revascularization — the growth of new blood vessels toward implanted follicles — is a critical determinant of graft survival, reduced scalp blood flow from stress-induced vasoconstriction creates a less favorable vascular environment for graft integration.
A third mechanism involves cortisol’s immunosuppressive effects. The immune system plays a specific role in hair follicle cycling, with immune cell populations in the scalp contributing to the regulation of follicle transition between growth phases. Chronic cortisol elevation disrupts this immune regulation in ways that can impair the normal hair growth cycle — adding another pathway through which sustained stress affects follicle function.
The Procedural Stress of the Hair Transplant Itself
Before discussing post-procedure stress, it is worth acknowledging that the hair transplant procedure itself constitutes a significant physiological stressor — one that directly contributes to the shock loss that occurs in the weeks following.
The physical stress of extraction, handling, and implantation of follicular units produces a biological stress response in the affected follicles. The disruption of the follicle’s blood supply from the moment of extraction, the ischemic period before revascularization is established, and the inflammatory response to the tissue trauma of the procedure all contribute to the follicle’s entry into telogen — the mechanism of shock loss. This is why shock loss is a universal feature of hair transplant recovery regardless of how gentle the surgical technique is: the stress of the procedure itself reliably triggers the follicle’s stress response.
Understanding that the procedure creates a baseline of physiological stress for the follicles — stress that they are working to recover from in the weeks and months after — contextualizes why additional stress during the recovery period is particularly significant. Follicles that are already navigating procedural stress recovery are more vulnerable to the hair-cycle-disrupting effects of additional psychological and physiological stress than follicles in normal resting state.
Psychological Stress During Recovery: The Anxiety Paradox
One of the most practically significant — and most underappreciated — stress dynamics in hair transplant recovery is what might be called the anxiety paradox: the recovery process itself generates anxiety that, if poorly managed, can interfere with the biological processes it’s being anxious about.
The anxiety sources that arise during hair transplant recovery are specific and predictable. Shock loss anxiety — the distress of watching transplanted and adjacent native hair shed in the first weeks after the procedure — is the most common and most intense. Patients who weren’t fully prepared for shock loss encounter what looks like accelerating hair loss rather than improving coverage, and the psychological response is frequently alarm, regret, and fear that the procedure hasn’t worked or has made things worse. This anxiety, if sustained and intense, generates the cortisol response that can compound the biological shock loss through the mechanisms described above.
Progress monitoring anxiety — the stress of daily evaluation of a slowly developing result against hoped-for benchmarks — creates sustained low-level anxiety throughout the waiting period of months two through five. Patients who check their scalp multiple times daily, who photograph and compare in unflattering lighting conditions, who compare their month-three appearance to clinic galleries of twelve-month results — are generating repeated cortisol responses to the absence of progress they’re hoping to see but that biology isn’t yet ready to provide.
Social anxiety during the visible phases of recovery — the weeks when swelling, scabbing, and then shock loss make the procedure evident — adds situational stress particularly for patients who didn’t plan adequate time away from social or professional obligations. The stress of concealing a healing procedure in contexts where concealment is difficult compounds the biological stresses of recovery with the psychological stress of social performance.
The practical significance of these anxiety sources is not that they will definitively cause graft failure — the evidence for specific quantifiable effects of psychological stress on graft survival in the post-transplant context is limited. The significance is that sustained anxiety creates a cortisol environment that is genuinely less favorable for the biological processes of recovery than a calmer state would produce, and that the anxiety is itself largely preventable through appropriate pre-procedure information and expectation-setting.
Telogen Effluvium: The Specific Stress-Shock Loss Interaction
The most direct interaction between stress and hair transplant outcomes is the potential for significant post-procedure psychological stress to trigger or extend telogen effluvium — shedding — beyond the shock loss that the procedure itself causes.
Procedural shock loss has a predictable timeline: shedding begins in weeks two through four, peaks around weeks four to eight, and gradually resolves as follicles return to anagen over the following months. This biological pattern is driven by the procedural stress and occurs on a timeline determined by follicle biology rather than patient behavior.
Additional significant psychological stress during this period — sustained high-cortisol states from work pressure, relationship difficulties, financial anxiety, or the shock loss anxiety itself — can trigger additional telogen entry in follicles that would otherwise have cycled independently of the procedure’s effects. The result can be more pronounced or more prolonged shedding than the procedural shock loss alone would have produced.
This is not a theoretical risk. Telogen effluvium from psychological stress has been well-documented in clinical literature across many decades, and the two-to-three-month delay between a stressor and the resulting shedding — reflecting the follicle’s lag time between telogen entry and visible shedding — means that stress experienced during the early recovery period can produce visible shedding during the month-three-to-five period when patients are anxiously watching for new growth rather than ongoing loss.
The practical implication is specific: minimizing sustained psychological stress during the first three to four months of recovery — the period during which stress is most likely to produce additional telogen entry — is a genuinely useful strategy for optimizing the recovery trajectory, not a generic wellness recommendation.
Sleep: The Most Undervalued Recovery Tool
Sleep quality is one of the most direct connections between stress and hair transplant recovery — and it deserves specific treatment because the relationship operates in both directions. Stress impairs sleep. Poor sleep generates stress. And both stress and poor sleep independently affect the biological processes that determine how well the recovery proceeds.
During sleep, the body allocates resources to tissue repair and cellular regeneration in ways that are less available during waking hours. Growth hormone — which is primarily secreted during deep sleep — supports tissue repair, protein synthesis, and cell proliferation throughout the body including in the scalp. Adequate deep sleep provides the biological environment in which the cellular repair of extraction and implantation wounds proceeds most efficiently.
Sleep deprivation elevates cortisol levels — a direct hormonal consequence of insufficient rest that has been documented across many studies. Patients who are sleeping poorly during the recovery period, whether from pain, anxiety, the elevated-head sleeping requirement of the first few days, or independent sleep difficulties, are operating with chronically elevated cortisol that creates exactly the less-favorable follicle environment described earlier in this guide.
The specific challenge of sleep in the first week of recovery — the requirement for head elevation at approximately 45 degrees to minimize swelling — disrupts normal sleep architecture for many patients and can produce sleep quality deficits that contribute to cortisol elevation in the early critical healing period. Planning the sleep arrangement carefully before the procedure — testing pillow arrangements or recliner positions, preparing for the first night specifically — reduces this disruption and supports better sleep quality in the period when sleep’s contribution to healing is most significant.
Pain management in the first nights — taking prescribed analgesics proactively rather than waiting until pain is significant — also directly supports sleep quality by preventing pain-related waking that both disrupts sleep architecture and activates stress responses.
Physical Stress: Exercise, Activity, and the Cortisol Response
The activity restrictions following a hair transplant are typically framed in terms of graft dislodgement risk — avoiding the increased scalp blood flow and physical compression risks that strenuous activity creates in the first two weeks. But the stress physiology of physical activity is an additional reason that gradual return to exercise matters for recovery outcomes.
Intense exercise — particularly heavy resistance training — activates the same hormonal stress axis as psychological stress, generating cortisol as part of the physiological response to physical challenge. For healthy individuals not recovering from surgery, this exercise-induced cortisol spike is a normal part of the training response and is followed by recovery processes that have net positive effects. In the context of early post-transplant recovery, the acute cortisol elevation from intense exercise adds to the biological stress environment that recovering follicles are navigating.
This provides additional physiological rationale beyond the physical compression and bleeding risks for the recommendation to avoid strenuous exercise for the first two to four weeks: the hormonal stress response to intense exercise creates a less favorable recovery environment beyond the physical risks at the scalp level.
Conversely, moderate exercise — walking, light movement — has well-documented stress-reducing effects through endorphin release and cortisol reduction. The gradual return to moderate physical activity from weeks two to three, before progressing to more intense training from weeks four to six, supports both the physical recovery timeline and the psychological stress management that benefits recovery overall.
The Nutritional Stress Connection
Stress and nutrition interact in the post-transplant recovery context in ways that compound their individual effects on recovery outcomes.
Chronic psychological stress increases the body’s consumption of specific micronutrients — particularly B vitamins, vitamin C, and magnesium — that are also directly relevant to hair follicle function and wound healing. A patient under sustained stress during recovery may deplete these nutrients faster than dietary intake replaces them, creating functional deficiencies that compromise recovery even when dietary intake appears adequate.
Stress also affects appetite and food choices in ways that can compromise post-transplant nutritional support. Many people under stress either reduce their food intake — producing the caloric restriction that triggers additional telogen effluvium — or shift toward processed, high-sugar foods that don’t provide the protein, iron, zinc, and vitamins that recovery depends on. The stress-nutrition interaction creates a compounding pathway where psychological stress produces nutritional compromise that then compounds the biological effects of the stress itself.
The practical implication is that nutritional attention and stress management are not independent recovery protocols — they reinforce each other. Adequate nutritional support during stressful periods of recovery helps buffer the cortisol response; stress management that improves sleep and reduces anxiety supports better appetite regulation and more consistent dietary quality.
Scalp Blood Flow: The Vascular Stress Connection
One of the most direct physical mechanisms through which stress affects hair transplant recovery is through scalp circulation. The vasoconstriction — narrowing of blood vessels — that accompanies cortisol elevation and sympathetic nervous system activation reduces blood flow to peripheral tissue including the scalp.
In the post-transplant context, where revascularization of transplanted grafts — the growth of new capillaries toward implanted follicles from the surrounding tissue — is a primary determinant of graft survival, reduced scalp blood flow from sustained stress creates a less favorable vascular environment for this critical process. Grafts in tissue that is well-perfused, with robust circulation delivering oxygen and nutrients efficiently, establish their new blood supply more robustly than those in tissue where stress-induced vasoconstriction is reducing perfusion quality.
This is one of the mechanisms through which activities that support good circulation — adequate hydration, moderate exercise after the first weeks, smoking avoidance — benefit graft survival beyond their other direct effects. Conversely, it is one of the mechanisms through which the vasoconstriction of chronic stress, nicotine, and significant alcohol intake — all of which activate vasoconstriction through overlapping mechanisms — create less favorable vascular conditions for graft integration.
Managing Stress During Recovery: Practical Strategies
Understanding the biological mechanisms through which stress affects hair transplant recovery translates into a specific set of practical management strategies — not generic wellness advice, but targeted interventions that address the specific pathways through which stress interferes with recovery.
Pre-procedure information that prevents shock loss panic is the most high-leverage stress management intervention available. Patients who understand the shock loss timeline specifically — not just “some hair may fall out” but “the transplanted hair will shed in weeks two through eight, the scalp will look sparse through months two to four, new growth begins around months three to five” — respond to shock loss with comprehension rather than alarm. The difference in cortisol response between “this is exactly what I was told to expect” and “something has gone wrong” is meaningful and entirely preventable through good pre-procedure communication. This guide, and others like it, serve that function — converting anticipated experiences from stressors into expected milestones.
Establishing a structured assessment schedule reduces progress monitoring anxiety by replacing continuous unstructured checking with intentional monthly photographic review. Daily scalp checking under unflattering bathroom lighting generates repeated stress responses to absence of visible progress that biology isn’t yet providing. Monthly consistent-condition photography documents genuine trend without the daily negative reinforcement of overhead-lit bathroom mirrors showing the worst-case representation of an early recovery stage.
Sleep optimization is directly relevant to recovery outcomes through the growth hormone and cortisol mechanisms described above. Planning the first week’s sleep arrangement before the procedure day, taking prescribed pain management proactively, maintaining consistent sleep and wake times, and limiting screen exposure before sleep all support the sleep quality that recovery depends on.
Moderate physical activity from week two to three provides stress-reducing benefits — endorphin release, cortisol reduction, improved sleep quality — while respecting the physical recovery timeline. The transition from no exercise in the first two weeks to light walking and movement in weeks two to three, building to moderate exercise in weeks three to four, and returning to full activity from weeks four to six, is calibrated to both the physical recovery timeline and the stress management timeline.
Social planning around recovery reduces the situational stress of managing visible recovery signs in social or professional contexts. Planning adequate time away from high-visibility social and professional obligations during the most visible phases — the first two weeks of swelling and scabbing — eliminates a category of stress that would otherwise be added to the baseline of recovery stress. Patients who plan their procedure timing around quieter social periods, and who prepare honest but minimal explanations for people who may notice changes, navigate this phase with significantly less stress than those who manage the visible recovery period reactively.
Avoiding alcohol during recovery serves a stress management function in addition to its direct biological effects on protein synthesis and vascular function. Many patients use alcohol as a stress management strategy in everyday life. During recovery, this strategy becomes counterproductive — the stress relief of the first drink is followed by sleep disruption, cortisol elevation, and the specific biological interferences with healing described elsewhere. Alternative stress management strategies — moderate exercise when permitted, adequate sleep, social connection, structured relaxation practices — serve the stress management function without the recovery-compromising effects.
Maintaining social connection and support has well-documented cortisol-buffering effects. Patients who have at least one person who knows about the procedure and can provide genuine support — not false reassurance but actual accompaniment through the uncertainty of recovery — consistently navigate the psychological challenges of recovery better than those who manage it in complete secrecy. The choice of whether to disclose the procedure is entirely personal, but complete secrecy adds the additional stress of social performance during a recovery period that is already psychologically demanding.
When Stress Management Requires Professional Support
For most patients, the stress of hair transplant recovery is a manageable period of temporary psychological discomfort that resolves as the result develops. For a smaller proportion of patients, the recovery period intersects with existing anxiety, depression, or body dysmorphic concerns in ways that exceed the capacity of self-management strategies.
Patients who find that anxiety about the recovery is significantly affecting daily function — disrupting sleep beyond the first week, impairing concentration at work, dominating social interactions, producing persistent intrusive thoughts about the procedure — are experiencing a level of stress that warrants professional support. A brief course of cognitive behavioral therapy, professional counseling, or in some cases short-term pharmacological support for anxiety is appropriate when recovery stress reaches this level of functional impact.
The threshold for seeking professional support should be functional impact rather than the generic standard of “serious enough” — anxiety that is interfering with daily life is appropriate to address with professional help regardless of whether it seems proportionate to the situation. The recovery period is genuinely challenging psychologically, and accessing appropriate support is not an overreaction to manageable discomfort but a reasonable response to distress that is affecting quality of life.
At Hairpol, post-procedure support includes specific guidance about the psychological aspects of recovery — including what to expect at each phase — because patients who understand the psychological landscape of recovery navigate it with significantly better outcomes than those who encounter each phase without preparation. The biology of the procedure and the psychology of the recovery are not separate concerns. They are two aspects of the same experience, and addressing both with equal seriousness produces the best complete result.
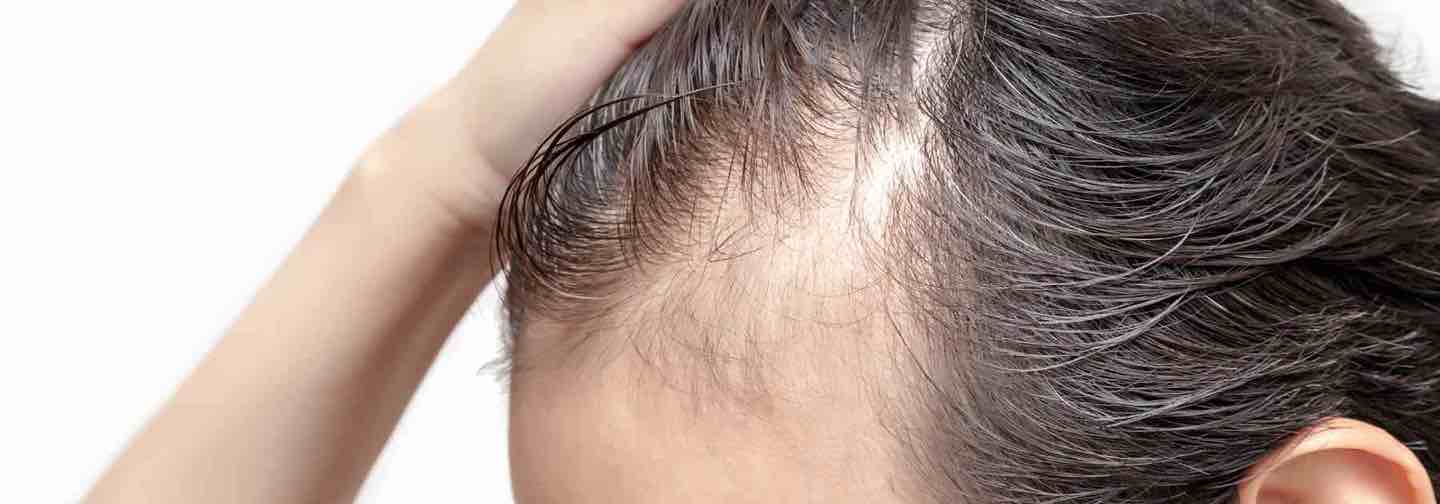
The Honest Summary
Stress affects hair transplant recovery through specific biological mechanisms — cortisol-mediated promotion of telogen entry, vasoconstriction that reduces scalp blood flow during the critical revascularization period, disruption of sleep that impairs growth hormone-mediated tissue repair, and nutritional depletion that compounds the direct effects of stress on follicle function. These mechanisms are real, biologically plausible, and directly relevant to the recovery period.
The magnitude of stress effects on graft survival is not definitively quantified in the research literature in the way that, say, the effects of iron deficiency or smoking are quantified. But the biological mechanisms are established, the direction of effects is consistently toward less favorable recovery conditions, and the practical strategies for managing stress during recovery carry essentially no downside risk. Stress management during hair transplant recovery is therefore worth taking seriously as a genuine component of the recovery protocol — not because anxiety will certainly doom a procedure, but because reducing it creates a meaningfully more favorable biological environment for the result being grown.
The recovery period is a test of patience as much as it is a biological process. Understanding specifically what is happening at each stage, why it looks the way it does, and what the evidence-based timeline for improvement actually is — transforms the experience from one driven by anxious uncertainty to one navigated with comprehension. That transformation is itself the most effective stress management strategy available for the specific challenges of hair transplant recovery.
Frequently Asked Questions (FAQ)
Can stress cause a hair transplant to fail?
Stress does not cause hair transplant failure in the sense of eliminating graft survival entirely, but it does create biological conditions that are less favorable for the recovery processes that determine how well grafts survive and how robustly growth emerges. The primary mechanism is cortisol — the body's main stress hormone — which promotes follicle entry into telogen (the resting phase), inhibits growth factors that support active hair growth including IGF-1 and FGF, and causes vasoconstriction that reduces scalp blood flow during the critical period of revascularization when transplanted grafts are establishing their new blood supply. Sustained high stress during recovery creates a cortisol environment that is genuinely less supportive of graft integration and eventual anagen re-entry than a calmer physiological state would produce. The magnitude of this effect varies between patients and the evidence for its specific quantification in the hair transplant context is limited — but the biological mechanisms are real, the direction of effects consistently unfavorable, and the practical strategies for stress reduction carry no downside risk. Stress management is a legitimate recovery protocol component for a hair transplant patient, not merely a generic wellness recommendation.
Why does stress cause hair loss after a hair transplant?
Stress causes hair-related changes after a hair transplant through the same mechanism that produces telogen effluvium in everyday life — elevated cortisol promoting premature follicle entry into the telogen (resting) phase. The hair transplant procedure itself is a significant physiological stressor that reliably triggers shock loss — follicle telogen entry in response to the trauma of extraction and implantation — which is why shock loss is universal in hair transplant recovery. Additional psychological stress during the recovery period can compound this procedural shock loss by triggering further telogen entry in follicles that would otherwise have cycled independently of the procedure's effects. The resulting shedding typically manifests two to three months after the stressor — the biological lag time between telogen entry and visible shedding — which means stress during early recovery can produce visible effects during the month-three-to-five window when patients are anxiously watching for new growth. Understanding this timeline helps distinguish stress-related additional shedding from the expected procedural shock loss and contextualize it as a temporary biological response rather than evidence that the procedure has failed.
Does anxiety about shock loss make it worse?
Yes — the anxiety that shock loss commonly generates can compound the biological shock loss through the cortisol mechanism that underlies stress-related hair shedding. Shock loss — the shedding of transplanted and adjacent native hair in weeks two through eight after a hair transplant — is driven by the procedural stress of extraction and implantation. When shock loss triggers significant anxiety in patients who weren't fully prepared for it, that anxiety generates sustained cortisol elevation that can promote additional telogen entry in follicles beyond those directly affected by the procedural stress. This creates a feedback cycle where shock loss generates anxiety, anxiety generates additional shedding, and additional shedding generates more anxiety. The most effective intervention for breaking this cycle is the one that prevents it from forming: thorough pre-procedure information that specifically describes the shock loss timeline — hair sheds in weeks two through eight, the scalp looks sparse through months two to four, new growth begins around months three to five — so that the experience of shock loss triggers recognition rather than alarm. Patients who encounter shock loss as confirmation of expected recovery progress have a dramatically different cortisol response than those who encounter it as evidence that something has gone wrong.
How does sleep affect hair transplant recovery?
Sleep is one of the most directly impactful and most underemphasized variables in hair transplant recovery. During deep sleep, the body secretes growth hormone — which supports tissue repair, protein synthesis, and cell proliferation throughout the body including at the donor extraction and recipient implantation sites — in ways that are less available during waking hours. Adequate deep sleep provides the biological environment in which cellular healing proceeds most efficiently. Sleep deprivation independently elevates cortisol levels, creating the same less-favorable follicle environment that psychological stress produces through the same hormonal pathway. Patients sleeping poorly during recovery — whether from pain, anxiety, the head-elevation requirement of the first nights, or independent sleep difficulties — operate with chronically elevated cortisol that compromises the recovery process. Practical sleep optimization for the recovery period includes: planning the head-elevation sleeping arrangement before the procedure day; taking prescribed pain management proactively to prevent pain-related waking; maintaining consistent sleep and wake times; limiting screen exposure before sleep; and addressing any pre-existing sleep difficulties with appropriate strategies. The investment in good sleep quality during recovery returns directly in better healing conditions and reduced cortisol-mediated recovery interference.
Can work stress during hair transplant recovery affect results?
Yes — sustained work stress during hair transplant recovery creates the cortisol environment that is directly relevant to recovery outcomes through the mechanisms described above. Chronic work pressure, high-stakes deadlines, difficult interpersonal dynamics, and the sustained cortisol elevation these generate are biologically equivalent to other forms of psychological stress in terms of their effects on follicle biology, scalp blood flow, and sleep quality. The practical implication is that planning the procedure timing around periods of lower professional pressure — rather than during particularly demanding work phases — gives the recovery period a more favorable stress environment. For patients whose professional circumstances don't allow flexibility in timing, deliberate stress management during the recovery period — protecting sleep, limiting unnecessary additional stressors, building in genuine recovery time — serves a genuine biological purpose rather than being merely a lifestyle preference. The specific period of highest biological significance for stress management is the first three to four months of recovery, when follicles are most vulnerable to additional telogen entry from stress-elevated cortisol and when the revascularization process determining graft survival is most actively proceeding.
Does exercise help or hurt hair transplant recovery?
The relationship between exercise and hair transplant recovery changes across the recovery timeline in ways that make the simple question require a nuanced answer. In the first two weeks, strenuous exercise creates multiple direct risks: increased blood pressure and scalp blood flow elevating bleeding risk from fresh wounds; sweating across healing graft sites increasing infection risk; and the cortisol response to intense physical challenge adding to the biological stress environment of early recovery. Strenuous exercise should be avoided during this period. From weeks two to three, moderate exercise — walking, light movement — becomes actively beneficial. Moderate physical activity reduces cortisol, releases endorphins that reduce psychological stress, and improves sleep quality — all of which support the recovery process through the stress-biology mechanisms described in this guide. The gradual return to full exercise intensity from weeks four to six respects both the physical recovery timeline and the stress management considerations: the hormonal stress response to intense exercise is most relevant during early recovery when follicles are most vulnerable, and becomes progressively less significant as integration strengthens. Moderate exercise through months two to six — the waiting period and early growth emergence — actively supports recovery by managing the anxiety and stress that the waiting period generates.
How can I manage stress during hair transplant recovery?
Managing stress during hair transplant recovery involves specific strategies targeted at the biological pathways through which stress affects recovery outcomes. The highest-leverage intervention is pre-procedure information that specifically describes the shock loss timeline and the complete recovery sequence — patients who understand what each phase looks like and why respond to expected experiences with recognition rather than anxiety-generating alarm. Establishing a structured monthly assessment schedule rather than daily scalp checking reduces the repeated stress responses to absence of progress that biology isn't yet providing. Optimizing sleep through head-elevation planning, proactive pain management, and consistent sleep timing directly addresses the cortisol mechanism through which poor sleep compromises recovery. Moderate exercise from weeks two to three provides cortisol-reducing and endorphin-releasing benefits while respecting the physical recovery timeline. Maintaining social connection with at least one supportive person who knows about the procedure provides documented cortisol-buffering effects. Avoiding alcohol as a stress management strategy removes the sleep disruption and protein synthesis inhibition that make it counterproductive during recovery despite its short-term anxiolytic effect. And for patients whose anxiety is significantly affecting daily function — disrupting sleep, impairing concentration, producing persistent intrusive thoughts — professional support through counseling or cognitive behavioral therapy is appropriate rather than being reserved as a last resort.
When should I be worried about stress affecting my hair transplant?
Stress is worth specific attention in hair transplant recovery when it is sustained rather than episodic, and when it is affecting sleep quality, appetite, or daily function — because these are the conditions under which its biological effects on cortisol, scalp blood flow, and follicle cycling are most consequential. Brief acute stressors — a difficult day at work, a single night of poor sleep — have limited impact on recovery outcomes. Chronic sustained stress — weeks of elevated cortisol from unresolved anxiety, ongoing sleep disruption, severe appetite disturbance — creates the biological conditions that genuinely affect the recovery environment. Specific warning signs that stress during recovery warrants more active management include: persistent sleep disruption beyond the first week due to anxiety rather than physical discomfort; daily function significantly impaired by recovery anxiety; intrusive thoughts about the procedure dominating waking hours; using alcohol regularly to manage recovery anxiety; or noticing shedding that extends significantly beyond the expected shock loss timeline. When stress reaches the level of functional impairment, professional support — counseling, cognitive behavioral therapy, or medical assessment — is appropriate and represents a legitimate component of recovery management rather than an overreaction. The goal is not the elimination of all stress, which is neither achievable nor necessary, but the prevention of sustained high-cortisol states during the three to four months of recovery when follicle biology is most sensitive to the hormonal environment.