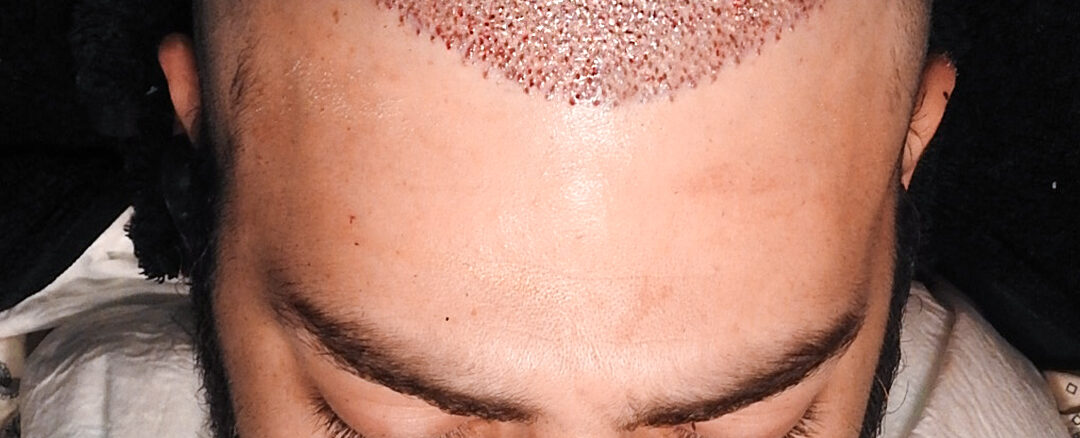
The procedure is done. You’re back at the hotel or home, and for the first time, you’re alone with your thoughts — and a head full of tiny grafts that cost you real money, real time, and a fair amount of trust.
The first week after a hair transplant is where most of the anxiety lives. Not because it’s medically complicated, but because it looks alarming if you don’t know what’s coming. Redness, swelling, crusting, tightness — none of it signals failure. All of it is part of how your scalp heals.
This guide walks through what actually happens in the first seven days, what’s normal, what needs attention, and how to protect the result you’ve just invested in.
Why the First Seven Days Matter More Than People Realize
The grafts placed during your hair transplant aren’t locked in immediately. For roughly the first 72 hours, they are anchored by the body’s early healing response — thin fibrin clots that form around each follicle. They’re holding, but they’re not secure the way they’ll be a week later.
This is why the first days aren’t about rest in the casual sense. It’s about protecting a biological process that’s happening with or without your cooperation. The more you understand what’s going on under the surface, the easier it is to follow aftercare without feeling like you’re guessing.
By the end of day seven, the grafts are physically secure. The scabs are forming or already softening. The most vulnerable window is closing. What you do in those seven days has a direct effect on how your hair transplant results develop over the next twelve months.
Day 1: The Immediate Post-Procedure Period
You’ll likely feel a combination of mild soreness, tightness across the recipient area, and a strange awareness of your own scalp. Local anesthesia wears off gradually, and as it does, you may notice:
- A dull pressure or stinging in the donor area (usually the back of the head)
- Tightness across the transplanted zone
- Mild sensitivity to touch
- Occasional itching as the skin begins its initial response
None of this requires strong pain management for most patients. Over-the-counter pain relief is usually sufficient. Your clinic will provide specific instructions on what to take and what to avoid — particularly blood-thinning medications like aspirin or ibuprofen, which can increase the risk of minor bleeding.
Sleeping position matters enormously on day one. You need to keep your head elevated — ideally at a 45-degree angle — to prevent swelling from pooling in the forehead. Some patients use a travel pillow or stack two pillows to keep the neck supported. The goal is to avoid direct contact between the recipient area and any surface, which means sleeping on your back, not your side.
Don’t touch the grafts. Don’t scratch. Don’t examine them too closely by pressing fingertips against the scalp. It feels counterintuitive when you want to check everything, but contact in this first phase is unnecessary risk.
Day 2: Swelling Begins
Most people are surprised by day two. The donor area looks manageable. But swelling often appears — starting at the forehead and sometimes moving down toward the eyes and nose by day three.
This is not an allergic reaction. It’s not an infection. It’s the fluid from the tumescent solution used during the procedure redistributing downward by gravity. The swelling is temporary and typically peaks on days two through four before resolving on its own.
Cold compresses applied to the forehead — not the recipient area — can help reduce the swelling. The key word is forehead. Nothing cold, nothing pressing directly on the transplanted scalp.
You may also notice that the donor area looks pink and slightly raw. This is expected. The follicles were extracted from this zone, and the skin there needs the same careful treatment as the top of the scalp.
Keep activity minimal. Walk slowly if needed. No bending forward at the waist, which increases blood pressure to the scalp. No lifting anything heavy. The goal is to keep your head calm and your blood pressure stable.
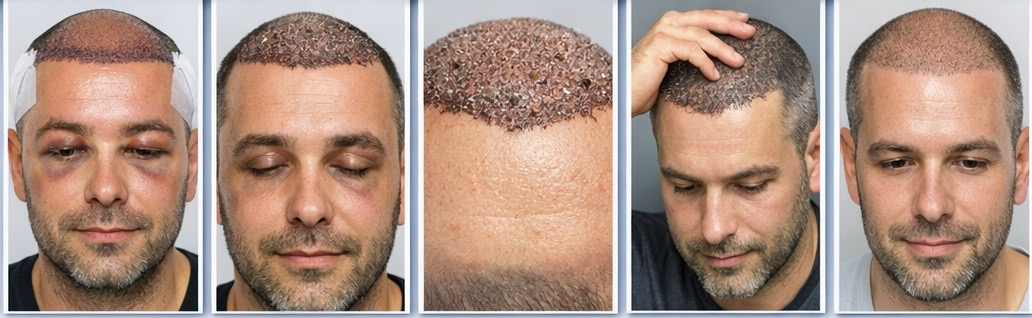
Day 3: Scabs Begin to Form
By the third day, small scabs are forming around each graft. This is the body doing exactly what it should — creating a protective layer over each implanted follicle while healing begins underneath.
The scabs can look dense and slightly alarming if you were expecting something cleaner. Some people describe the scalp at this stage as looking like a dotted texture or a rough patch of skin. This is normal, and more importantly, it’s temporary.
What you must not do is pick, scratch, or try to remove scabs. Each scab is connected to a graft. Pulling a scab before it’s ready to release naturally carries real risk of pulling the follicle with it. Graft loss in the first days is almost always caused by physical interference, not by something going wrong internally.
If your clinic has prescribed a saline spray or specific lotion, continue applying it exactly as directed. Keeping the area lightly moisturized reduces tightness without softening the scabs prematurely.
The donor area is usually healing faster by this point. Redness there begins to settle, and any tightness across the back of the head eases gradually.
Day 4: The Swelling Window
For many patients, day four is the peak of visible swelling. The forehead may look noticeably puffier, and some people see mild bruising under the eyes.
This is entirely within the normal hair transplant recovery process and requires no intervention beyond keeping the head elevated and staying hydrated. The swelling resolves on its own as the fluid disperses and is reabsorbed.
This is also the day when the psychological side of recovery often becomes more present. You may look in the mirror and feel like something is wrong — the swelling, the scabs, the redness, the unfamiliar appearance of your own head. This is a very common experience, and it passes.
Understanding the hair transplant timeline helps here. Day four is not a preview of your result. It is the deepest point of the healing trough, and what you’re seeing now has almost nothing to do with what your hair will look like in six months.
Stay off social media comparisons. Don’t search for “day 4 hair transplant” photos and compare them to professional after shots. The comparison is meaningless and only feeds unnecessary anxiety.
Day 5: Scabs Consolidate and Healing Accelerates
The swelling usually begins to ease. The scabs on the recipient area are now more established. Redness in the donor area may be noticeably reduced.
If your clinic has introduced a gentle washing routine — typically starting around day three or four and continuing through the first week — you’ll be rinsing carefully with a diluted shampoo solution and lukewarm water. The washing technique matters as much as the product. Gentle pouring of water rather than rubbing, no fingernails, no direct pressure.
The first wash can feel nerve-wracking. It helps to remember that gentle washing at this stage is recommended by the clinic precisely because it supports healing — it keeps the area clean, prevents buildup, and begins the slow, controlled process of softening scabs naturally.
By day five, most patients report that the initial soreness has reduced significantly. The donor area often feels more like a mild sunburn than active soreness. The recipient area still feels tight but less sensitive to the air around it.
Day 6: A Quieter Day in the Process
Day six tends to feel steadier. The dramatic swelling of days two through four has eased for most patients. The scabs are present but no longer worsening. The scalp is settling into a stable state.
This is when some people make the mistake of feeling well enough to return to normal life too quickly — resuming exercise, going to the gym, returning to physical work, or spending extended time outdoors without protection.
Avoid all of these. Sweat on the scalp during the first week increases infection risk and can interfere with healing. Direct sun exposure on the newly transplanted area can damage grafts that are still establishing. Heavy physical activity raises blood pressure and can cause minor bleeding in the recipient zone.
A short walk is fine. A light routine indoors is fine. Anything that raises your heart rate significantly or exposes your scalp to direct elements is not.
If you’re traveling back home from a clinic abroad — something common for patients who choose a hair transplant in Istanbul — day six is often the travel day. Wear a loose-fitting hat that doesn’t press on the recipient area. Avoid direct sun at the airport. Stay hydrated. Don’t let the logistics push you into lifting heavy luggage or rushing in a way that stresses the scalp.
Day 7: The First Week Closes
By the end of day seven, the grafts are considered physically secure. The fibrin anchoring from the first days has been replaced by early tissue integration. You’re past the most vulnerable window.
The scabs are still present but often beginning to look less rigid. Redness in both the recipient and donor areas has reduced for most patients compared to day one. The scalp may still feel tight, and you may still notice sensitivity — but the acute phase of recovery is behind you.
This is not when results appear. The hair you’re seeing now — if any is visible above the scalp — is not representative of your final outcome. Many patients enter a phase over the following weeks where the transplanted hairs shed. This is called shock loss or the shedding phase, and it is entirely expected. The follicles remain intact underground even when the visible hair falls out.
The first week is only the beginning of the hair transplant timeline. Real density and coverage develop between months three and twelve. The work you do in week one creates the foundation for what grows later.
What You Should and Shouldn’t Do: A Clear Summary
Getting through the first week successfully comes down to a short list of consistent habits.
Do:
- Sleep on your back with your head elevated for the full first week
- Follow the clinic’s washing instructions exactly — not earlier, not more aggressively
- Use the prescribed sprays or moisturizers as directed
- Stay hydrated and eat normally
- Wear loose, button-up clothing that doesn’t go over your head
- Rest and keep activity genuinely minimal
Don’t:
- Touch, pick, scratch, or rub the recipient area
- Bend forward at the waist repeatedly
- Exercise, swim, or do anything that causes sweating
- Expose the scalp to direct sun without protection
- Drink alcohol, which can thin the blood and affect healing
- Pull clothing over your head in a way that catches on the scalp
- Judge your result based on how anything looks this week
A Note on Warning Signs
Most of what happens in the first week is normal and expected. But there are genuine signs that something needs attention.
Contact your clinic if you notice:
- Significant bleeding that doesn’t stop with gentle pressure
- Increasing pain rather than gradually decreasing discomfort
- Fever, chills, or general illness symptoms
- Discharge or unusual smell from the recipient or donor area
- A graft that appears to have been completely dislodged
These are not common. But they are the situations where contacting your clinic immediately is the right move, not waiting to see if it resolves.
The Mindset That Makes the First Week Easier
There’s a version of the first week where you check your scalp every thirty minutes, photograph every change, and spend hours reading about everything that can go wrong. That version makes the week feel very long and very stressful.
There’s another version where you understand that your scalp is healing exactly as it should, you follow the aftercare without improvising, and you let the process happen.
The second version produces the same biological result. It just feels significantly better.
Your hair transplant is not in danger every time the scalp itches or a scab looks darker than yesterday. These are surface events happening on top of a healing process that, for the overwhelming majority of patients who follow proper aftercare, proceeds exactly as planned.
Trust the clinic that performed your procedure. Follow their specific instructions — which may differ slightly from general guidelines depending on technique, graft count, and your individual scalp characteristics. And give your body the quiet, undramatic week it needs to start building the result you came for.
The first seven days are not a preview of the outcome. They’re the foundation of it.
Frequently Asked Questions (FAQ)
How long does swelling last after a hair transplant?
Swelling after a hair transplant typically begins on day two and peaks between days three and four. It usually resolves on its own within five to seven days without any medical intervention. The swelling is caused by tumescent fluid used during the procedure redistributing downward by gravity — it is not a sign of infection or allergic reaction. Keeping the head elevated at roughly 45 degrees during sleep and applying cold compresses to the forehead (never to the recipient area) helps reduce the severity and duration of swelling during the first week of recovery.
Can I touch my scalp in the first week after a hair transplant?
Direct contact with the recipient area should be avoided entirely during the first week after a hair transplant. In the first 72 hours, grafts are anchored only by a thin fibrin seal and have not yet integrated into the surrounding tissue. Touching, scratching, or pressing the scalp during this window can physically dislodge a graft, and a dislodged graft is permanently lost. Even after scabs begin forming on day three, picking or rubbing the recipient area carries the risk of pulling a follicle out along with the scab. The safest approach is to treat the entire transplanted zone as off-limits to touch until your clinic confirms the grafts are secure.
When can I wash my hair normally after a hair transplant?
Gentle washing typically begins around days three to four after a hair transplant, following the specific protocol provided by your clinic. During the first week, washing means carefully pouring lukewarm water over the scalp and applying a diluted, gentle shampoo solution without any rubbing, scrubbing, or fingernail contact. Normal washing — with regular pressure and technique — is not appropriate until the scabs have fully resolved and the scalp surface has healed, which typically occurs around the end of the second week. Following your clinic's exact washing instructions rather than general guidance is important, as protocols can vary depending on technique and individual healing.
Is it normal to see redness after a hair transplant in the first week?
Yes, redness in both the recipient area and the donor area is entirely normal during the first week after a hair transplant. It is a standard part of the skin's inflammatory healing response and does not indicate infection or poor graft survival. Redness in the donor area typically begins fading by days three to five. Redness in the recipient zone often persists longer — sometimes several weeks — particularly in patients with fair or sensitive skin. Avoiding direct sun exposure, following the prescribed aftercare routine, and keeping the scalp clean all support faster resolution of post-procedure redness.
What happens if I sleep on my side after a hair transplant?
Sleeping on your side in the first week after a hair transplant risks bringing the recipient area into direct contact with the pillow, which can create sustained pressure on grafts that are still in the early stages of integration. In the first 72 hours when grafts are most vulnerable, prolonged lateral contact is the most common cause of accidental graft disturbance during sleep. Sleeping on your back with the head elevated at approximately 45 degrees is the recommended position for the full first week. A travel neck pillow placed around the neck helps prevent unconscious rolling to the side during sleep and is one of the most practical tools for maintaining the correct position throughout the night.
Will I see hair growth in the first seven days after a hair transplant?
Visible hair growth does not occur in the first seven days after a hair transplant. The transplanted follicles are in the early stages of establishing a new blood supply and have not yet re-entered the active growth phase. Any hair shafts visible above the scalp during the first week are the original shafts that were attached to the grafts at the time of implantation — they are not new growth. Most of these shafts will shed over the following weeks as the follicles enter a temporary resting phase known as shock loss. Genuine new growth from transplanted follicles typically begins appearing between months three and five of the hair transplant timeline.
Can I travel by plane in the first week after a hair transplant?
Traveling by plane during the first week after a hair transplant is generally possible but requires specific precautions. The most common travel window for international patients is around days five to seven, once the initial swelling has begun to reduce and the scabs are more established. During travel, a loose-fitting hat that doesn't press directly on the recipient area provides protection from sun exposure and incidental contact. Staying well hydrated on the flight supports the vascular conditions that healing tissue depends on. Avoiding overhead luggage that requires lifting heavy bags, rushing through airports, or extended direct sun exposure at departure or arrival are all practical precautions that reduce unnecessary stress on a scalp still in its first week of recovery.
When should I contact my clinic during the first week after a hair transplant?
Most of what occurs in the first week after a hair transplant — redness, swelling, scabbing, tightness, and mild soreness — is normal and does not require clinical intervention. However, there are specific signs that warrant contacting your clinic promptly. These include significant bleeding from the recipient or donor area that does not stop with gentle pressure, pain that is increasing rather than gradually reducing, fever or chills suggesting a systemic response, any discharge or unusual smell from the scalp, or a graft that appears to have been completely dislodged. These situations are uncommon in patients following proper aftercare, but when they occur they require professional assessment rather than a wait-and-see approach. Your clinic's contact details should be accessible throughout the first week for exactly this reason.