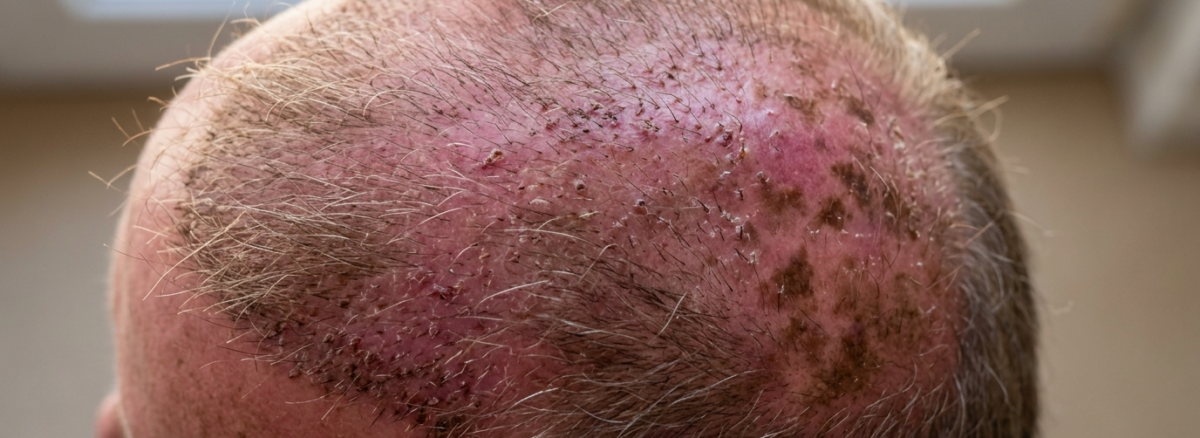
Most patients think about sun protection in general terms — wear a hat, stay out of direct sun, don’t burn. The advice sounds simple and the reasoning seems obvious. But the actual relationship between UV exposure and hair transplant recovery is more specific and more consequential than the general guidance suggests, and understanding exactly what sunlight does to a healing scalp at different stages of recovery changes how seriously patients take the precautions.
This isn’t about avoiding a tan. It’s about understanding that UV radiation interacts with healing tissue, vulnerable follicles, and pigment-producing cells in ways that can affect both the recovery process and the permanent quality of the result. Some of those effects are temporary and manageable. Others are not.
What UV Radiation Actually Does to Skin
Before getting into what sunlight does specifically to a transplanted scalp, it’s worth understanding what UV radiation does to skin in general, because the mechanisms are the same, just operating on tissue that is simultaneously healing from a surgical procedure.
Ultraviolet radiation from the sun arrives at the skin’s surface in two primary forms. UVB rays are shorter wavelength and are primarily responsible for sunburn. They penetrate into the outer layers of the epidermis and cause direct DNA damage to skin cells, triggering the inflammatory response that produces redness, pain, and peeling. UVA rays penetrate more deeply into the dermis and are primarily responsible for longer-term skin damage, premature aging, and the degradation of collagen in the deeper layers of the skin.
Both types are relevant to hair transplant recovery, but they matter at different stages and for different reasons.
UV radiation suppresses the local immune response of the skin. This is partly why people feel the relaxing warmth of sun exposure — the immune system in the skin is temporarily downregulated by UV. In the context of a healing surgical wound, this immune suppression removes some of the body’s capacity to protect against bacterial colonization and manage the inflammatory phases of healing correctly.
UV also stimulates melanocytes — the pigment-producing cells in the skin — to produce more melanin in response to radiation exposure. This is what causes tanning. In healing skin, this melanocyte stimulation can produce uneven pigmentation responses, because the cells in recently traumatized tissue don’t respond to UV the same way intact skin does. The result can be hyperpigmentation — patches of darker skin — that develop over the recipient or donor areas after sun exposure during the healing period.
Heat from sun exposure also matters independently of UV radiation. The scalp is a heat-sensitive environment during recovery, and sustained heat exposure increases blood flow to the scalp in ways that can affect swelling and inflammation during the early healing phases.
The First Two Weeks: The Most Critical Sun Exposure Window
The first fourteen days after a hair transplant represent the period of highest vulnerability to sun-related damage. During this window, the recipient area has open healing wounds around each graft, the skin barrier is compromised, and the transplanted follicles are in the process of establishing their initial blood supply through revascularization.
Direct sun exposure during this period creates multiple simultaneous problems.
UV radiation on unprotected healing skin in the recipient zone interferes with the inflammatory cascade that is managing the early phases of wound healing. The body’s healing process requires a specific sequence of inflammatory and anti-inflammatory phases to proceed correctly. UV-induced immune suppression disrupts this sequence, potentially slowing the closure of the small wounds around each graft and increasing susceptibility to infection.
The heat component of direct sun exposure raises scalp temperature, which increases local blood flow. In the first week when the fibrin seal anchoring grafts is still establishing, increased blood flow from heat exposure adds unnecessary physiological stress to a system that needs stability. Patients who spend significant time in direct sun during the first week risk increased swelling and a more difficult early healing course than those who stay out of direct sunlight entirely.
Sunburn during the first two weeks is a genuinely serious concern. A sunburned scalp during the early healing phase is not just uncomfortable — it represents a UV-induced inflammatory injury layered on top of a scalp that is already managing the inflammatory demands of surgical healing. The combined inflammatory load is harder for the tissue to manage and can compromise the microenvironment that the newly implanted grafts need to begin revascularization and integration.
The donor area is equally vulnerable during this period. The extraction sites are healing puncture wounds, and the skin there responds to UV exposure with the same vulnerability as the recipient zone. Patients who protect the recipient area with a hat but leave the back of the head exposed to sun are protecting one healing zone while exposing another.
The practical guidance for weeks one and two is unambiguous: avoid direct sun exposure entirely when possible. When outdoor exposure is unavoidable, cover the entire scalp with a loose, non-compressing hat or cap that doesn’t put pressure on the recipient area, and keep sun exposure as brief as possible.
Weeks Two to Four: Healing Progresses but Vulnerability Continues
After the two-week mark, the surface healing of the recipient area has progressed significantly. The small wounds around each graft have closed, the scabs have resolved, and the skin barrier is largely restored. The follicles are integrating into their new tissue environment. The acute vulnerability of the first two weeks has reduced, but the scalp is not yet in a state where normal sun exposure is appropriate.
The primary concern that continues through this phase is pigmentation. The skin in the recipient and donor areas is still in an active healing phase during weeks two to four, and melanocytes in this tissue remain reactive in ways that differ from fully healed skin. UV exposure during this period can trigger hyperpigmentation responses that produce patchy darkening of the scalp skin in the treated areas.
This hyperpigmentation is not permanent in most cases, but it can persist for several months and can affect the appearance of the scalp during the period when patients are hoping to see consistent improvement. In patients with darker skin tones, post-inflammatory hyperpigmentation from UV exposure during the healing period can be more pronounced and take longer to resolve than in lighter-skinned patients.
The redness that many patients experience in the recipient area during the first several weeks is also affected by sun exposure. UV radiation makes redness more pronounced and harder to resolve by maintaining a level of inflammation in the skin that would otherwise be settling. Patients who minimize sun exposure during this phase typically find their redness resolves faster than those who don’t.
Continued hat use during direct outdoor sun exposure is appropriate through weeks two to four. The hat requirements become slightly less critical than in weeks one and two — the window of acute graft vulnerability has closed — but pigmentation and redness management remain valid reasons to maintain sun protection through this phase.
The Shedding Phase and Sun Exposure
The shedding phase, which typically occurs between weeks two and eight, introduces a specific consideration about sun exposure that is worth understanding separately.
When transplanted hair sheds during this phase, the scalp in the recipient area becomes more exposed than it was before the procedure. Patients with longer hair often have some natural UV protection from the hair shaft simply shading the scalp. In the shedding phase, this natural protection is reduced or eliminated, leaving the scalp more directly exposed to UV radiation than it normally would be.
This increased exposure vulnerability coincides with a period when the follicles are in telogen, resting and cycling through their reset phase underground. While the follicles in telogen are less actively metabolically demanding than those in anagen, the scalp skin above them is still in the middle of its healing process, and UV exposure during this period carries the same pigmentation risks described above.
The practical implication is that sun protection during the shedding phase needs to account for the reduced natural UV protection from hair coverage. Patients who might otherwise rely on their existing hair to provide some scalp shading need to recognize that this protection is temporarily reduced and adjust accordingly.
Sunscreen on a Healing Scalp: What to Know
The question of whether to use sunscreen on the healing scalp after a hair transplant comes up frequently and deserves a direct answer, because the guidance is more nuanced than simply applying whatever sunscreen is normally used on the rest of the body.
In the first two weeks, sunscreen should not be applied directly to the recipient area. The skin barrier is compromised, and the chemical compounds in most sunscreens — including many fragrance and preservative ingredients — can cause irritation or allergic response when applied to healing wounds. The approach during this period is physical protection through hats and avoidance rather than topical sunscreen.
From around weeks three to four onward, mineral sunscreens — those using zinc oxide or titanium dioxide as the active ingredient rather than chemical UV filters — can typically be applied to the healed recipient area. Mineral sunscreens sit on top of the skin and reflect UV radiation rather than being absorbed into the skin, which makes them less likely to cause irritation on skin that has recently healed. They should be applied gently without rubbing, and any sunscreen should be chosen without fragrances or alcohol that could irritate recently healed skin.
Chemical sunscreens containing oxybenzone, avobenzone, or similar compounds are better avoided on the recipient area until the scalp is fully healed, typically from around month two or three. These compounds are absorbed into the skin and can cause contact irritation on recently healed tissue in some patients.
For the donor area, the same progression applies. Physical protection in the first two weeks, mineral sunscreen from weeks three to four, gradual introduction of standard sunscreen products from month two onward.
Long-Term UV Protection and the Permanent Result
The sun protection guidance for hair transplant recovery is typically framed around the acute healing phase, and many patients assume that once recovery is complete, normal sun exposure resumes without specific concern. This is partly true but not completely.
The skin of the scalp, once hair has grown back substantially, receives significant natural UV protection from the hair itself. Hair provides meaningful shading of the scalp — this is partly why scalp skin ages differently from facial skin that is chronically UV-exposed. For patients with good density outcomes from their hair transplant, the growing hair gradually takes over much of the natural sun protection that was compromised during the shedding phase.
For patients whose results include lower density in certain zones — the crown being the most common area where this applies — the scalp skin in those zones continues to receive more UV exposure than skin beneath dense hair coverage. Chronic UV exposure on the crown scalp over years and decades contributes to skin aging and pigmentation changes in that area. This is worth factoring into long-term scalp care habits, particularly for patients in high-UV climates.
The follicles themselves can be affected by chronic UV exposure over the long term. UV radiation has been associated with oxidative stress in hair follicles, and patients in extreme UV environments — those spending long hours in direct equatorial sun or at high altitude — are worth considering for ongoing scalp sun protection as a general practice beyond the acute recovery period.
Practical Situations That Require Planning
The sun exposure guidance becomes most practically challenging in specific real-life situations that patients encounter during their recovery period. Each requires slightly different management.
Beach and pool environments combine direct sunlight, reflective surfaces, heat, and often water exposure in a way that makes them among the highest UV-risk settings during recovery. UV radiation reflects off water and sand, meaning that time at the beach delivers significantly more UV exposure to the scalp than the same duration of time in a shaded urban environment.
Outdoor work that involves sustained exposure to direct sun requires practical planning around hat use and scheduling during the recovery period. Patients whose jobs take them outdoors for extended periods may need to consider wide-brimmed hats or headwear that provides more complete scalp coverage than a typical baseball cap.
Travel to high-altitude destinations increases UV intensity significantly. UV radiation increases by approximately four percent for every 300 meters of altitude, meaning that patients traveling to mountain destinations during recovery are exposed to meaningfully higher UV levels than sea-level equivalents.
Hot climates that combine high UV with high ambient temperature create a double challenge — the UV protection requirements of the healing phase combined with the heat management concerns of the early recovery period. Patients recovering in these environments should prioritize staying indoors during peak UV hours, typically between 10am and 4pm, and treat hat use as non-negotiable when outdoor exposure is required.
Hats: What Type, When, and How
The practical tool most patients use for sun protection during hair transplant recovery is a hat, and the choice and use of headwear during recovery is worth being specific about because not all hats provide equivalent protection or are equally safe for the healing scalp.
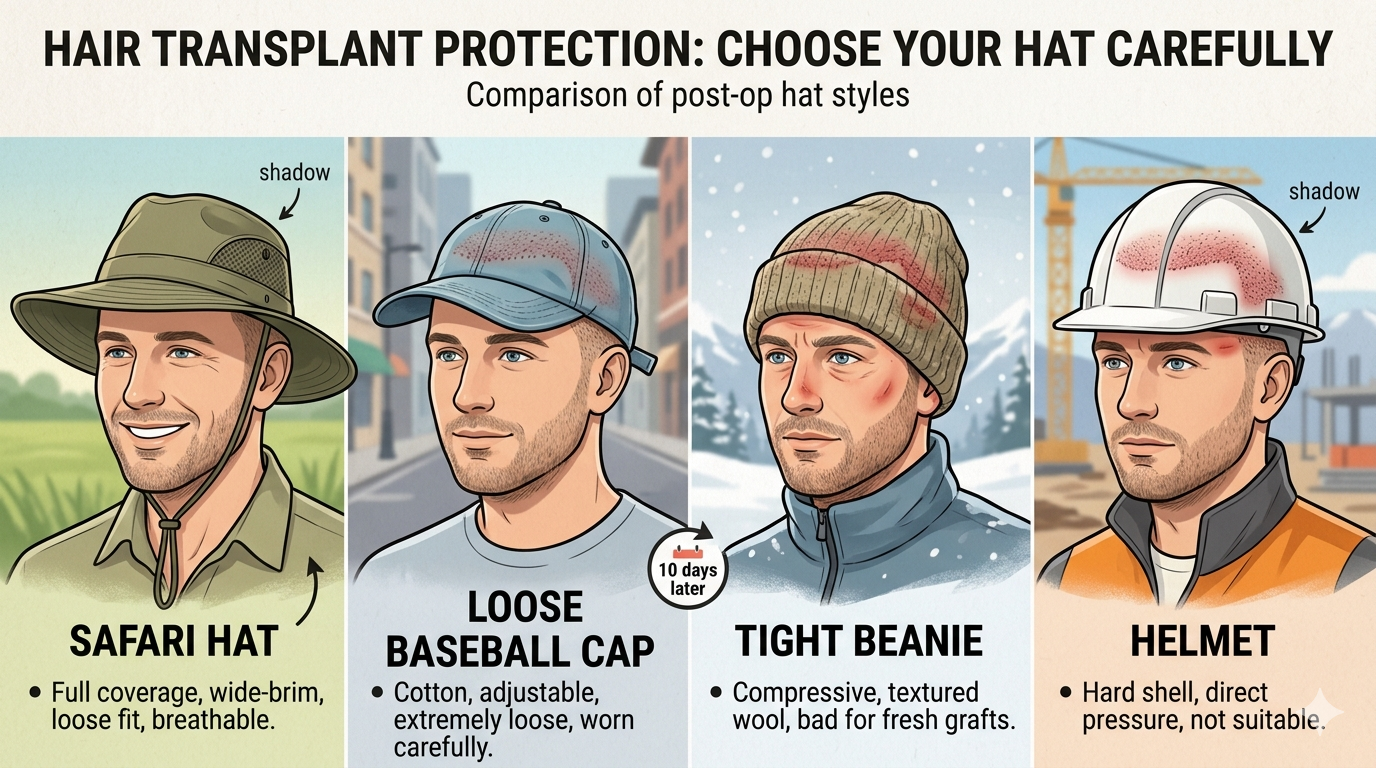
In the first ten days, any hat worn over the recipient area must be loose enough to avoid direct contact with the grafts. A hat that sits directly on the transplanted zone can create pressure that disturbs healing grafts, and in the first week when grafts are most vulnerable, hat selection matters beyond just UV protection. Loose, wide-brimmed hats that create a brim shadow without touching the recipient area are ideal during this early phase. Baseball caps that contact the frontal hairline area directly are not appropriate in the first week.
From week two onward, the graft security concern diminishes and hat selection becomes primarily about UV protection and comfort. Baseball caps that provide reasonable frontal coverage are appropriate from this point. Wide-brimmed sun hats provide better overall scalp protection, including the crown and sides, which a baseball cap leaves exposed.
Tight headwear that compresses the scalp, including beanies, tight fitted caps, and headbands, should be avoided through the first month regardless of UV exposure concerns, because compression on the healing scalp is uncomfortable and potentially counterproductive to the healing process.
The duration of hat requirements for sun protection is generally considered most critical through the first three months. After this point, the scalp has fully healed and the follicles are in active growth. Standard sun protection practices that apply to any sun-sensitive scalp are appropriate from month three onward.
The Connection Between Sun Exposure and Scarring
Both the recipient area and the donor area involve healing wounds, and scar formation in these areas is affected by UV exposure during the healing period in a way that is underappreciated by most patients.
UV exposure on healing wounds stimulates melanocyte activity in the scar tissue, which can result in hyperpigmented scars that are darker than the surrounding skin. In the recipient area, this hyperpigmentation affects the scalp skin between grafts and can make the scalp appear less uniform in color during the early stages of hair growth. In the donor area, hyperpigmented puncture scars are more visible if the hair is worn short and can take longer to fade when the healing period included significant UV exposure.
Conversely, UV protection during the healing period supports the formation of flatter, less pigmented scars that are less visually apparent as the hair grows. This is a consistent finding across surgical wound healing generally, and it applies to the small wounds of hair transplant recovery as directly as it does to any other surgical scar.
The practical implication is that sun protection during recovery is not only about protecting the follicles. It actively supports the cosmetic quality of the healing scalp skin, which is the surface against which the growing hair will eventually be seen.
The Simple Version
The reasoning behind sun avoidance after a hair transplant comes down to a short list of specific concerns that apply with different intensity at different phases of recovery.
In the first two weeks, direct sun exposure risks interfering with the immune-mediated healing process, disturbing the thermal environment that healing grafts need, and potentially causing sunburn on skin that is already managing significant healing demands. Physical avoidance and hat protection are the approach.
In weeks two to four, the acute vulnerability has reduced but the pigmentation risk from UV exposure on recently healed skin remains real. Hat use during direct sun exposure and avoidance of peak UV hours is appropriate.
From month two onward, the scalp has healed and standard sun protection practices apply. Mineral sunscreen can be used on the scalp skin between months two and three. Long-term consideration of scalp UV protection is worth maintaining as a general habit, particularly in high UV environments and for patients with lower density in certain zones.
The sun will be there when recovery is complete. Protecting the scalp during the window when it’s healing costs very little relative to the quality of the result it helps preserve.
Frequently Asked Questions (FAQ)
Why should I avoid sun exposure after a hair transplant?
Sun exposure after a hair transplant carries several specific risks that go beyond ordinary sunburn concerns. UV radiation suppresses the local immune response of healing skin, interfering with the inflammatory cascade that manages the early phases of wound healing and increasing susceptibility to infection. Heat from sun exposure raises scalp temperature and increases blood flow to the scalp in the early weeks when the fibrin seal anchoring grafts still needs stability. UV exposure during the healing period also stimulates melanocytes in a way that can produce patchy hyperpigmentation — uneven darkening of the scalp skin in the recipient and donor areas. Together these effects can compromise both the recovery process and the long-term cosmetic quality of the result.
How long should I avoid direct sun after a hair transplant?
Direct sun avoidance is most critical during the first two weeks after a hair transplant, when the recipient area has open healing wounds around each graft and the skin barrier is compromised. During this period, outdoor exposure should be minimized entirely when possible, and a loose, non-compressing hat should be worn when outdoors. Through weeks two to four, the acute graft vulnerability has reduced but pigmentation risk from UV exposure on recently healed skin remains, and hat use during direct outdoor exposure is still appropriate. Hat use for UV protection is generally considered most critical through the first three months, after which the scalp has fully healed and standard sun protection practices are sufficient.
Can I use sunscreen on my scalp after a hair transplant?
Sunscreen should not be applied directly to the recipient area during the first two weeks after a hair transplant — the skin barrier is compromised and chemical compounds in most sunscreens can cause irritation or allergic response when applied to healing wounds. Physical protection through hats and sun avoidance is the appropriate approach during this window. From around weeks three to four onward, mineral sunscreens using zinc oxide or titanium dioxide as the active ingredient can typically be applied gently to the healed recipient area — these reflect UV rather than absorbing into the skin, making them less likely to cause irritation. Chemical sunscreens containing oxybenzone or avobenzone should be avoided on the recipient area until the scalp is fully healed, typically from around month two or three.
What happens if my scalp gets sunburned after a hair transplant?
Sunburn on the scalp during the early healing phase after a hair transplant is a genuinely serious concern rather than just a comfort issue. A sunburned scalp in the first two weeks represents a UV-induced inflammatory injury layered on top of tissue that is already managing the significant inflammatory demands of surgical healing. The combined inflammatory load is harder for the tissue to manage and can compromise the microenvironment the newly implanted grafts need to begin revascularization and integration into surrounding tissue. Sunburn during this period can also disrupt the healing sequence of the small wounds around each graft, increasing susceptibility to infection and potentially affecting graft survival. If sunburn occurs during the first two weeks, contacting your clinic is appropriate rather than waiting to see how it resolves.
Does the shedding phase affect how vulnerable my scalp is to sun damage?
Yes — the shedding phase, which typically occurs between weeks two and eight after a hair transplant, increases scalp UV vulnerability in a specific way. When transplanted hair sheds during this phase, the scalp in the recipient area becomes more directly exposed to UV radiation than it normally would be. Patients with longer hair often have some natural UV protection from the hair shading the scalp — in the shedding phase, this natural protection is reduced or eliminated. This increased exposure coincides with a period when the scalp skin is still completing its healing process and carries the same hyperpigmentation risks as the earlier recovery phase. Sun protection during the shedding phase should account for this reduced natural hair coverage.
Does sun exposure affect the donor area as well as the recipient area?
Yes — the donor area at the back and sides of the scalp is equally vulnerable to UV exposure during the healing period following a hair transplant. The extraction sites in the donor area are healing puncture wounds, and the skin there responds to UV exposure with the same vulnerability as the recipient zone in terms of infection risk, hyperpigmentation, and scar quality. Patients who protect the recipient area with a hat but leave the back of the head exposed to sun are protecting one healing zone while leaving another unprotected. The same sunscreen progression applies to both areas: physical protection in the first two weeks, mineral sunscreen from weeks three to four, and standard sunscreen products from around month two or three. The back of the scalp and neck may have less natural coverage from certain hat styles and should receive deliberate sun protection attention.
How does sun exposure affect scarring after a hair transplant?
UV exposure during the healing period significantly influences the cosmetic quality of scar formation in both the recipient area and the donor area after a hair transplant. UV exposure on healing wounds stimulates melanocyte activity in scar tissue, which can produce hyperpigmented scars that are darker than the surrounding skin. In the recipient area, this hyperpigmentation affects scalp skin between grafts and can create uneven coloration during the early stages of hair growth. In the donor area, hyperpigmented puncture scars are more visible when hair is worn short and can take longer to fade. Conversely, consistent UV protection during the healing period supports the formation of flatter, less pigmented scars that are less visually apparent as the hair grows — meaning sun protection during recovery actively improves the cosmetic quality of the healing scalp, not only the follicle outcomes.
What type of hat should I wear after a hair transplant for sun protection?
Hat selection after a hair transplant changes across the recovery phases. In the first ten days, any hat worn must be loose enough to avoid direct contact with the grafts — a hat that sits directly on the transplanted zone can create pressure that disturbs healing grafts. Loose, wide-brimmed hats that create shade without touching the recipient area are ideal during this phase. Baseball caps that contact the frontal hairline directly are not appropriate in the first week. From week two onward, graft security concerns diminish and hat selection becomes primarily about coverage and comfort — wide-brimmed sun hats provide better protection for the crown and sides that a baseball cap leaves exposed. Tight headwear including beanies, fitted caps, and headbands should be avoided through the first month because compression on the healing scalp is counterproductive regardless of UV protection considerations.