Among the adjunctive treatments that clinics offer around hair transplant procedures, PRP therapy — platelet-rich plasma — has become one of the most commonly recommended and most commonly misunderstood. Patients encounter it in two forms: as a pre-operative or intraoperative treatment administered during the transplant procedure itself, and as a post-operative series of sessions in the months following surgery. The claims made for it range from the modest and defensible to the extravagant and poorly supported, and the marketing around it is considerably more confident than the evidence base warrants.
This guide gives an honest account of what PRP is, what it does biologically, what the evidence actually shows about its effects in the hair transplant context, and how patients should think about whether it represents a worthwhile addition to their recovery and growth protocol. The answer is not a simple yes or no — it’s a nuanced assessment that requires understanding both what the treatment can plausibly contribute and where its limitations and uncertainties lie.
What PRP Actually Is
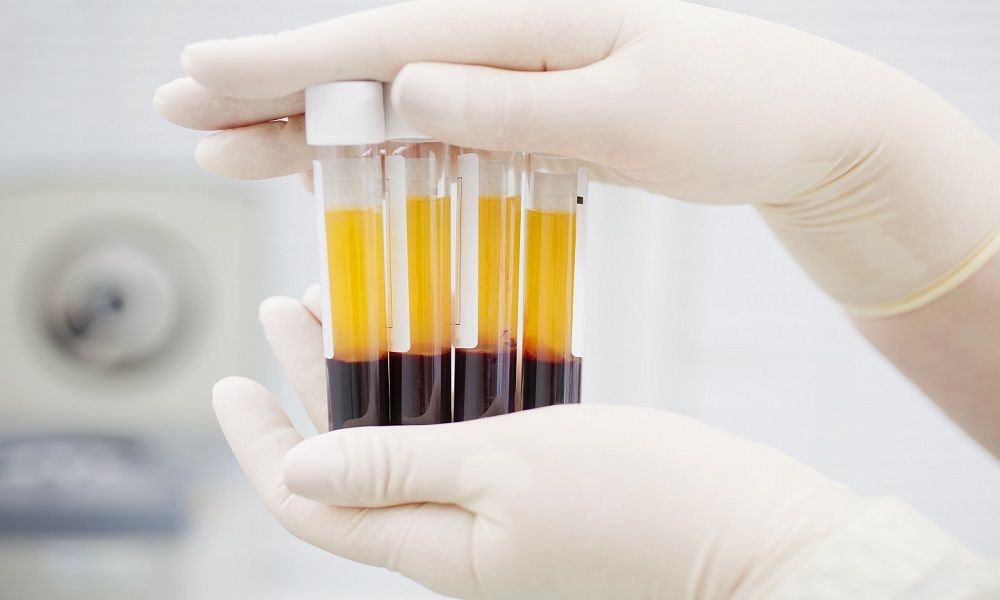
Platelet-rich plasma is produced from the patient’s own blood. A blood sample — typically 20 to 60 milliliters — is drawn, then placed in a centrifuge that separates the blood components by density. The centrifugation process separates red blood cells from plasma, and further fractionation concentrates the platelet-containing layer. The resulting PRP contains platelet concentrations several times higher than those found in normal circulating blood — typically three to five times the baseline platelet concentration, though the exact concentration varies with the processing system used.
Platelets are the blood cells primarily associated with clotting, but their role in tissue repair extends considerably beyond hemostasis. When platelets are activated — either by tissue injury in vivo or by calcium chloride or thrombin added during PRP preparation — they release a large collection of growth factors from granules stored in their cytoplasm. The growth factors relevant to hair follicle biology include:
Platelet-derived growth factor (PDGF), which stimulates cell proliferation and wound healing. Vascular endothelial growth factor (VEGF), which promotes the formation of new blood vessels — directly relevant to the revascularization of transplanted follicles. Insulin-like growth factor-1 (IGF-1), which supports cell survival and promotes the transition from telogen to anagen in hair follicles. Transforming growth factor-beta (TGF-β), which modulates inflammation and scar formation. Epidermal growth factor (EGF), which supports keratinocyte proliferation and wound healing. And fibroblast growth factor (FGF), which has direct roles in hair follicle cycling.
The biological logic of PRP in the hair restoration context is straightforward: concentrating these growth factors at the site of transplanted follicles provides a richer biochemical environment for the revascularization, integration, and eventual anagen re-entry of those follicles than they would experience in the absence of the treatment. This is a plausible mechanism, and it is the reason that PRP attracted serious scientific and clinical interest rather than being dismissed as pseudoscience.
The more complicated questions — whether this plausible mechanism translates into clinically meaningful improvements in outcomes, how large the effect size is when it does, and how consistently it is achieved across patients and protocols — are where the honest answer becomes considerably more nuanced.
The Evidence: What Studies Actually Show
The research literature on PRP for hair loss and hair transplantation is substantial — hundreds of studies published over the past two decades — but it is also heterogeneous, methodologically varied, and considerably less definitive than the confidence of clinical claims about PRP would suggest.
Studies examining PRP for androgenetic hair loss as a standalone treatment — in patients without a hair transplant — have generally found positive effects on hair density and thickness compared to placebo controls. Multiple systematic reviews and meta-analyses have concluded that PRP produces statistically significant improvements in hair count and hair thickness in treated areas. This is the most solid part of the evidence base.
The evidence specifically examining PRP in the context of hair transplantation — whether it improves graft survival, accelerates recovery, or enhances growth compared to transplant without PRP — is more mixed. Several randomized controlled trials have used split-scalp designs where one half of the recipient area received PRP treatment and the other half did not, allowing direct within-patient comparison. Results across these studies are inconsistent: some show significantly higher graft density in PRP-treated zones at three and six months; others show no statistically significant difference at twelve months when the comparison is made at full maturity.
This inconsistency reflects several genuine sources of variation that make the PRP literature difficult to interpret. The concentration of platelets in PRP varies significantly depending on the centrifugation protocol and processing system used — studies using lower-concentration PRP may find different results from those using higher-concentration preparations. The timing of PRP administration relative to the transplant — intraoperative versus multiple post-operative sessions — varies between studies. The outcome measures used vary — some studies measure hair count at three months, others at six, others at twelve, making direct comparison difficult. And many studies are small, with insufficient statistical power to detect real but modest effects.
The honest summary of the evidence is that PRP in the hair transplant context probably produces a real but modest positive effect on certain outcomes — particularly on the speed of early growth emergence and on the quality of the tissue environment during graft revascularization — but that the magnitude of this effect is smaller and less consistent than enthusiastic clinical claims suggest. The evidence does not support the position that PRP dramatically improves graft survival or final density in all or most patients. Nor does it support dismissing PRP as entirely without benefit.
The Intraoperative Application: PRP During the Transplant Itself
One of the most clinically supported applications of PRP in hair transplantation is its use during the procedure itself — either as a solution in which extracted grafts are stored while awaiting implantation, or as an injection into the recipient area before graft placement.
The rationale for graft storage in PRP is the most biologically compelling application. Extracted follicles are metabolically active but deprived of their blood supply from the moment of extraction until revascularization is established in their new location. During the time they spend outside the body — which can be several hours in large procedures — they are vulnerable to ischemic damage. PRP provides a growth-factor-rich medium that may better support follicle viability during this ex vivo period than standard saline or Ringer’s lactate storage solutions.
Several studies have found higher graft survival rates when PRP is used as a storage medium compared to standard solutions, though the effect is not universal across studies. The biological mechanism is plausible enough and the potential upside significant enough — graft survival is one of the primary determinants of final density — that many experienced clinics have incorporated PRP-based graft storage as part of their standard protocol.
Injection of PRP into the recipient area before graft placement — creating a growth-factor-enriched tissue environment at the sites where follicles will be implanted — is the other intraoperative application. The rationale is that elevated growth factor levels in the recipient tissue may support faster and more robust revascularization of implanted follicles. The evidence for this specific application is more variable than for graft storage, but the approach has become common in clinics that incorporate PRP into their transplant protocols.
Post-Operative PRP Sessions: The Evidence and the Rationale
The most common form in which patients encounter PRP after a hair transplant is as a series of post-operative sessions — typically three to four injections spaced four to six weeks apart during the first three to six months of recovery. This is where the claims about PRP supporting growth, reducing shock loss duration, and enhancing the early recovery process are most prominent — and where the evidence is most worth examining carefully.
The biological rationale for post-operative PRP sessions is that the growth factors delivered to the scalp support the follicles during the critical phases of their recovery: the telogen resting phase following shock loss, the revascularization process by which blood supply is re-established, and the eventual anagen re-entry when new hair production begins. By providing a periodic bolus of growth factors at the scalp level during this period, PRP may support these processes in ways that improve either the pace of recovery or the quality of growth when it eventually emerges.
The studies that have examined post-operative PRP sessions have found mixed results. Several have shown earlier emergence of new growth in PRP-treated patients — the months-three-to-five window when follicles begin exiting telogen appears somewhat earlier in some studies for patients who received post-operative PRP. This earlier emergence, if real and consistent, is a genuine benefit: it shortens the psychologically difficult waiting period and provides earlier visible evidence that the procedure is working.
Whether post-operative PRP produces meaningfully higher final density at twelve months — the clinically most significant outcome — is less consistently supported. Some studies show a density advantage for PRP-treated patients at twelve months; others show no significant difference at the endpoint that matters most for patient satisfaction. The most plausible interpretation of this mixed evidence is that PRP may accelerate the trajectory of early growth without substantially changing the final density endpoint — an effect that is genuinely valuable to some patients but less transformative than claims of “dramatically improved graft survival” would suggest.
PRP and Shock Loss: What the Evidence Suggests
One of the most common clinical claims about PRP in the post-transplant period is that it reduces the severity or duration of shock loss — the shedding of transplanted and adjacent native hair that occurs in weeks two through eight as follicles enter telogen in response to procedural stress.
The biological argument for this effect is that the growth factors in PRP — particularly IGF-1 and FGF, which have direct roles in supporting the anagen phase and in promoting the transition from telogen to anagen — may partially counteract the telogen-inducing stress signals that drive shock loss. By providing a local environment richer in anagen-supportive growth factors, PRP might maintain some follicles in anagen that would otherwise enter telogen, or might accelerate the recovery from telogen for follicles that do shed.
The evidence for this specific effect is suggestive but not definitive. Some studies report reduced hair count loss in the weeks following transplant for PRP-treated patients compared to controls. Others find no significant difference in the severity of shock loss. The inconsistency may reflect genuine biological variability — some patients’ follicles respond more to the growth factor environment than others — or it may reflect the measurement challenges of accurately counting hairs in a period characterized by active shedding and early regrowth simultaneously.
For native hair adjacent to the recipient zone — the DHT-sensitive follicles that experience stress-related telogen from the tissue disruption of the procedure — there is some evidence that PRP’s growth-factor environment supports faster recovery from this stress-induced telogen, potentially shortening the period during which these native hairs are absent from the overall coverage picture. This is a plausible and clinically relevant effect if it occurs consistently, though the evidence base for it is limited.
What PRP Cannot Do
Understanding the limitations of PRP is as important as understanding its potential benefits — particularly because the marketing environment around PRP in hair restoration tends to claim more than the evidence supports.
PRP cannot compensate for poor surgical technique. The primary determinants of graft survival are the quality of extraction and implantation — how carefully grafts were handled, how quickly they were implanted, how precisely the angles and density were executed. PRP provides a better biochemical environment for grafts that were well-handled; it cannot rescue grafts that were poorly handled or damaged during extraction.
PRP cannot produce hair in follicles that no longer exist. PRP has shown effects on existing follicles that are miniaturizing or in telogen. It has not demonstrated the ability to generate new follicles or to restore function to follicles that have completed their miniaturization cycle and are no longer present in the scalp. In the hair transplant context, this means PRP supports the follicles that were transplanted — it is not an alternative to having them transplanted in the first place.
PRP cannot reliably prevent all shock loss. As discussed, the evidence for PRP’s effect on shock loss severity is mixed. Patients who undergo PRP sessions with the expectation that they will not experience shock loss are likely to be disappointed. The more realistic expectation is that PRP may somewhat moderate the severity or duration of shock loss for some patients — not that it eliminates the biological phenomenon.
PRP results are not uniform across patients. Response to PRP varies significantly between individuals, likely reflecting differences in baseline growth factor content of platelets, differences in the scalp tissue environment, and individual variation in follicle responsiveness to growth factor stimulation. Some patients respond strongly to PRP; others show minimal benefit from identical protocols. This variability means that population-level evidence about PRP’s effects translates imperfectly to prediction of individual patient responses.
PRP is not a substitute for medical management. Finasteride and minoxidil have substantially stronger and more consistent evidence bases for managing ongoing androgenetic hair loss than PRP does. In the post-transplant context, the priority for patients who are candidates for medical management should be starting and maintaining finasteride and minoxidil — the native hair protection these medications provide over the medium and long term is more reliably significant than PRP’s effects on the early recovery period. PRP can complement these medications but should not be positioned as their replacement.
Protocol Variation: Why “PRP” Is Not a Single Treatment
One of the most significant challenges in evaluating PRP for hair transplantation is that “PRP” describes a category of treatments that vary considerably in ways that directly affect their biological potency and therefore their clinical outcomes.
The platelet concentration achieved varies by processing system and protocol — from less than two times baseline platelet concentration to more than ten times, depending on the centrifuge, centrifugation speed, and preparation method used. Growth factor content varies proportionally with platelet concentration, which means that studies using low-concentration PRP systems may find smaller effects than those using high-concentration systems — and that patients treated at clinics using lower-quality processing equipment receive a meaningfully less potent treatment than those at clinics using better systems, even when both treatments are called “PRP.”
The presence or absence of leukocytes — white blood cells — in the PRP preparation is another variable with clinical implications. Leukocyte-rich PRP (L-PRP) and leukocyte-poor or pure PRP (P-PRP) have different profiles of inflammatory and anti-inflammatory mediators that may produce different effects in scalp tissue. The evidence on whether L-PRP or P-PRP is preferable in the hair restoration context is not conclusive, but the distinction matters for interpreting results across studies that used different preparation protocols.
The number of sessions and the timing between them — typically three to four sessions at monthly intervals, but varying considerably between clinics — affects the cumulative growth factor exposure that treated follicles receive. A single session of high-quality PRP may or may not produce comparable effects to three sessions of lower-quality PRP.
These variations mean that asking “does PRP work for hair transplants?” is somewhat like asking “does medication work for headaches?” — the answer depends substantially on which PRP, administered with which protocol, in which patients, measured by which outcomes. This protocol heterogeneity is one of the primary reasons the evidence base is so difficult to interpret and why generic claims about PRP’s effectiveness are inadequately specific to be clinically useful.
PRP for Standalone Hair Loss (Without Transplant): A Stronger Evidence Base
While the evidence for PRP specifically in the hair transplant context is mixed, the evidence for PRP as a standalone treatment for androgenetic hair loss — in patients who have thinning but haven’t had a transplant — is somewhat more consistent. Multiple randomized controlled trials comparing PRP to placebo in androgenetic hair loss patients have found statistically significant improvements in hair count and hair thickness in PRP-treated groups.
For post-transplant patients who also have actively progressing androgenetic hair loss in native hair — which is common — PRP sessions in the months after the transplant may serve a dual purpose: supporting the recovery and growth of transplanted follicles while also providing some benefit to the native hair that continues to thin around the transplanted zone. In this context, the somewhat stronger evidence for PRP’s effects on native androgenetic hair adds to the rationale for post-operative PRP sessions beyond its transplant-specific effects.
This dual benefit — if present — makes PRP a somewhat more attractive option for transplant patients who are in the earlier stages of hair loss with substantial native hair that is actively miniaturizing, compared to patients whose loss is more advanced and who have less native hair that might respond to PRP’s effects on androgenetic progression.
The Practical Decision: Is PRP Worth It After a Hair Transplant?
Given the evidence base as honestly summarized, how should patients think about the decision to pursue PRP after a hair transplant?
The case for PRP is strongest when it is administered intraoperatively — particularly as a graft storage medium and as a recipient area injection during the procedure. The evidence for graft survival benefit in the storage medium application is more consistent than for post-operative sessions, and the additional cost and complexity are absorbed into the procedure rather than requiring separate sessions. Patients whose clinic incorporates intraoperative PRP as a standard protocol component are receiving the most evidence-supported application of the treatment.
The case for post-operative PRP sessions is weaker but not negligible. For patients who want to do everything reasonably available to support the best possible recovery — who are committed to the full protocol of medical management, nutritional optimization, and activity management, and for whom the additional time and cost of PRP sessions is acceptable — PRP represents a reasonable addition to that protocol. The probability that it produces some benefit is higher than the probability that it produces harm, and the magnitude of benefit, while smaller than enthusiastic claims suggest, is real in at least some patients.
For patients who are choosing between PRP and other elements of their post-transplant protocol, the priority ordering matters. Starting and maintaining finasteride — for candidates — is substantially more important for long-term result protection than PRP. Nutritional management of iron, vitamin D, zinc, and protein status is directly relevant to the speed and quality of anagen re-entry and has a stronger evidence base for specific effects on hair growth biology than PRP. These foundational elements should not be deprioritized in favor of PRP when resources — time, attention, cost — are limited.
Patients should be cautious of clinics that present PRP as a transformative addition that dramatically improves graft survival and doubles the speed of growth — claims that outrun the evidence. They should also be skeptical of PRP sessions priced at levels that suggest they are being treated as a significant revenue stream rather than an adjunctive support for the primary procedure. A clinic that is transparent about the evidence — including its limitations — and presents PRP as a potentially beneficial addition rather than as essential or transformative is giving patients more accurate information than one whose marketing claims exceed what the research supports.
At Hairpol, PRP is incorporated into the transplant protocol at the intraoperative stage — the application with the most consistent evidence for graft support — and discussed honestly with patients as a potentially beneficial post-operative adjunct whose effects are real but more modest than aggressive marketing typically suggests. Because patients who understand what PRP can and cannot do make better decisions about their recovery protocols than those who are responding to claims that overstate the evidence.
The Honest Summary
PRP therapy after a hair transplant sits in a genuinely intermediate position in the evidence hierarchy — more supported than most alternative or unproven treatments marketed in the hair restoration space, less definitively proven than the confident clinical claims about it suggest.
The biological mechanism is sound: concentrated growth factors delivered to transplanted follicles provide a more supportive biochemical environment for revascularization, telogen recovery, and anagen re-entry. The evidence shows real effects in some applications — particularly intraoperative graft storage — and suggestive but inconsistent effects for post-operative sessions on outcomes like early growth emergence. The evidence for dramatic improvements in final graft density at twelve months is less consistent.
The honest answer to whether PRP helps after a hair transplant is: probably yes, modestly, more reliably for some applications than others, not uniformly across all patients, not as dramatically as it is often marketed, and in a way that complements rather than replaces the foundational elements of medical management and nutritional optimization that have stronger and more consistent evidence bases for protecting long-term results.
That honest answer is the most useful one — for patients making informed decisions about their recovery protocols and for setting expectations that produce satisfaction rather than disappointment when results emerge on the timeline and at the density that hair biology, rather than optimistic marketing, actually delivers.
Frequently Asked Questions (FAQ)
What is PRP therapy and how does it work after a hair transplant?
PRP therapy — platelet-rich plasma — is a treatment produced from the patient's own blood. A blood sample is drawn and centrifuged to concentrate the platelet-rich layer, producing plasma containing three to five times the normal platelet concentration. When activated, platelets release growth factors including VEGF, PDGF, IGF-1, and FGF that support tissue repair, blood vessel formation, and hair follicle cycling. In the context of a hair transplant, PRP is used in two main ways: intraoperatively — as a storage medium for extracted grafts or as an injection into the recipient area before implantation — and post-operatively, as a series of scalp injections during the recovery period. The rationale is that delivering concentrated growth factors to transplanted follicles creates a more supportive biochemical environment for revascularization, telogen recovery, and anagen re-entry — the biological processes that determine how well and how quickly transplanted follicles establish themselves and begin producing new permanent hair.
Does PRP actually improve hair transplant graft survival?
The evidence that PRP improves graft survival in hair transplants is real but inconsistent across studies — stronger for some applications than others. The most consistently supported application is using PRP as a storage medium for extracted grafts while they await implantation. Several studies have found higher graft survival rates when grafts are stored in PRP compared to standard saline or Ringer's lactate solutions, reflecting PRP's growth factors supporting follicle viability during the ex vivo period when grafts lack blood supply. The evidence for graft survival improvement from recipient area PRP injections before implantation — creating a growth-factor-rich environment at implantation sites — is more variable. Studies comparing PRP-treated and untreated zones within the same patient using split-scalp designs show higher early density in PRP zones in some studies but no significant difference at twelve-month maturity in others. The honest summary is that PRP probably provides a real but modest benefit to graft survival — not the dramatic improvement that some clinical claims suggest, but real enough to justify its incorporation into surgical protocols by clinics that use quality processing systems.
Can PRP reduce shock loss after a hair transplant?
The claim that PRP reduces shock loss after a hair transplant has a plausible biological basis but mixed evidence. The growth factors in PRP — particularly IGF-1 and FGF — have direct roles in supporting the anagen phase and promoting the transition from telogen to anagen. By creating a local environment richer in anagen-supportive signals, PRP might partially counteract the telogen-inducing stress signals that drive shock loss or accelerate telogen recovery for follicles that do shed. Some studies report reduced hair count loss during the shock loss phase for PRP-treated patients compared to controls. Others find no significant difference in shock loss severity. The inconsistency may reflect genuine individual variation in follicle responsiveness to growth factor stimulation. The realistic expectation for PRP in this context is that it may moderately reduce the severity or duration of shock loss for some patients — not that it eliminates the biological phenomenon. Patients who expect PRP to prevent shock loss entirely are likely to be disappointed. Patients who understand it as a potential moderating influence are better positioned to evaluate their experience accurately.
How many PRP sessions are needed after a hair transplant?
The most common post-operative PRP protocol after a hair transplant involves three to four sessions spaced approximately four to six weeks apart during the first three to six months of recovery — the period when transplanted follicles are recovering from shock loss, completing the telogen resting phase, and beginning their anagen re-entry. This timing is designed to provide growth factor support during the phases of recovery most relevant to the eventual growth outcome. The specific number of sessions varies between clinics and is not definitively established by the evidence — the research literature uses protocols ranging from two to six sessions without a clear consensus on the optimal number. What the evidence does suggest is that multiple sessions across the first months are more likely to produce benefit than a single session, because the relevant biological processes — revascularization, telogen recovery, anagen re-entry — unfold over months rather than resolving at a single timepoint. Clinics with well-defined protocols and quality PRP processing systems are better positioned to deliver consistent results than those with variable preparation methods.
Is PRP better than finasteride for protecting hair transplant results?
No — finasteride has a substantially stronger and more consistent evidence base for protecting hair transplant results than PRP, and the two treatments address different aspects of the hair management picture. Finasteride protects results through its DHT-suppressing mechanism — slowing the progression of native hair loss in the years after the procedure, maintaining the native hair that provides density context for the transplanted zone, and reducing the rate at which additional sessions become necessary. This protective effect on native hair is the primary determinant of how the transplant result looks at five and ten years. PRP's most meaningful contributions are in the early recovery period — supporting graft viability, potentially moderating shock loss, and possibly accelerating early growth emergence. These are real but shorter-term and more modest in magnitude than finasteride's long-term native hair protection. For patients who are candidates for finasteride, starting and maintaining it consistently is the higher priority than PRP. PRP can complement finasteride as part of a comprehensive recovery protocol, but it should not be positioned as its replacement or equivalent in importance for long-term result protection.
Are all PRP treatments the same quality?
No — "PRP" describes a category of treatments that vary considerably in biological potency depending on the processing system and protocol used. The platelet concentration achieved varies from less than two times to more than ten times the baseline platelet concentration depending on the centrifuge, centrifugation speed, and preparation method. Since growth factor content varies proportionally with platelet concentration, patients treated with lower-concentration PRP preparations receive meaningfully less potent treatment than those receiving high-concentration PRP — even when both are called "PRP" in clinical discussion. The presence or absence of leukocytes in the preparation — producing leukocyte-rich versus pure PRP — creates different profiles of inflammatory mediators that may affect outcomes differently. The number and spacing of sessions adds further variation. These differences mean that comparing outcomes across clinics that use different PRP systems is difficult, and that generic claims about PRP effectiveness describe a range of treatments rather than a uniform intervention. Patients evaluating hair transplant clinics should ask specifically about the PRP processing system used and the platelet concentration achieved, rather than treating "we offer PRP" as a uniform quality indicator.
Should I get PRP before or after a hair transplant?
Both intraoperative and post-operative PRP have clinical rationale, and the two applications are not mutually exclusive. Intraoperative PRP — used as a graft storage medium during the procedure and as an injection into the recipient area before graft placement — has the most consistent evidence for graft survival support and is the application best integrated into the surgery itself rather than requiring separate sessions. Post-operative PRP sessions — typically three to four injections during the first three to six months of recovery — address the recovery period when transplanted follicles are completing telogen and beginning anagen re-entry. Clinics that incorporate intraoperative PRP as a standard protocol component are providing the most evidence-supported application. Post-operative sessions add potential benefit to early growth emergence and native hair support in patients with active androgenetic progression, though with more variable evidence for their effects on final density at twelve months. For patients making resource allocation decisions about their hair transplant protocol, the priority ordering should place finasteride and minoxidil for eligible patients ahead of post-operative PRP sessions, with PRP as a complementary addition rather than a foundational priority.
What are the risks of PRP therapy after a hair transplant?
PRP therapy after a hair transplant has a favorable safety profile compared to most medical interventions, primarily because it is derived from the patient's own blood — eliminating the risks of allergic reaction or disease transmission associated with donor materials. The most common side effects are injection-site reactions: temporary pain, swelling, and redness at injection points that typically resolve within one to two days. Rare reported complications include temporary scalp inflammation, hematoma formation at injection sites, and in very rare cases infection at the injection site — the same infection risk that attends any injection procedure. The risk of systemic adverse effects from PRP is low given its autologous nature. The more significant practical risk is not biological but economic and expectation-related: patients who pay for multiple PRP sessions expecting dramatic improvements in graft survival or elimination of shock loss based on overclaimed marketing may experience financial disappointment when results align with the more modest effects the evidence actually supports. Clinics that provide accurate, evidence-based information about what PRP can and cannot do allow patients to make decisions that reflect genuine informed consent rather than marketing-driven expectations.