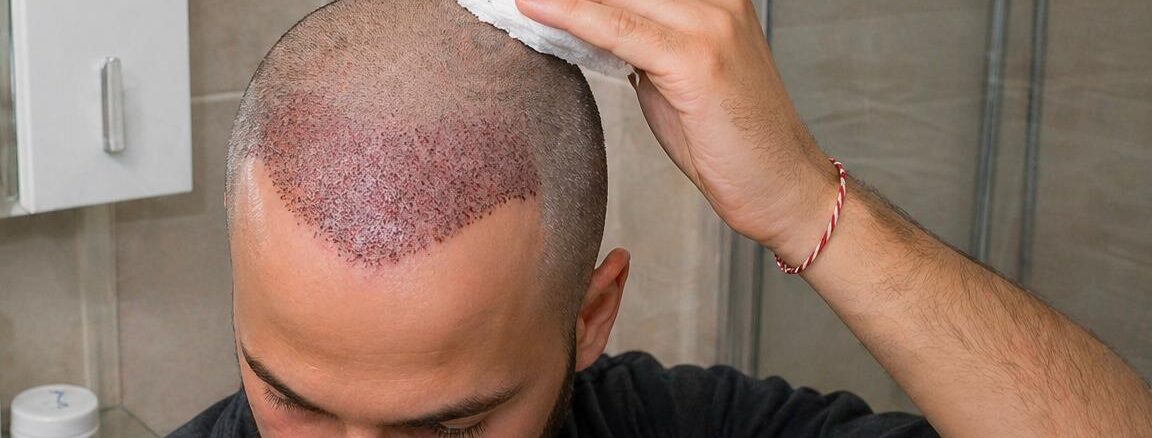
A hair transplant is a surgical procedure. Like all surgical procedures, its outcome depends not only on what happens in the operating room but on what happens in the weeks and months that follow. The difference between a well-executed procedure that produces the result it was designed to produce and the same procedure that falls short of its potential is, in a meaningful number of cases, the difference between patients who followed their aftercare instructions and those who didn’t.
This is not a generic warning. The aftercare instructions for a hair transplant are specific, grounded in the biological reality of how grafts integrate and heal, and directly linked to measurable outcomes — graft survival rates, scarring quality, infection risk, and the speed and completeness of the recovery. Understanding what specifically goes wrong when specific instructions are not followed — rather than simply being told that aftercare matters — gives patients both a clearer picture of the risks they’re managing and a better understanding of why each instruction exists.
This guide goes through the most important aftercare requirements and explains specifically what happens when they aren’t followed. Not as a scare tactic, but as the honest clinical information patients need to protect the investment they’ve made in their procedure.
The Biology of the Critical Window
Before getting into specific aftercare failures and their consequences, the most important biological context to understand is why the first fourteen days after a hair transplant are categorically different from everything that follows.
When grafts are implanted into the recipient area, they are initially held in place by a thin fibrin seal — the body’s initial clotting response to the implantation wounds. This fibrin seal provides the graft’s only anchoring mechanism for the first several days. It is strong enough to hold grafts in place under gentle, controlled conditions. It is not strong enough to withstand mechanical force, friction, water pressure, or the other stresses of normal daily activity.
Beginning around day four or five, the surrounding tissue begins forming early connections to the implanted grafts. By days ten to fourteen, most grafts have integrated sufficiently that the risk of physical dislodgement is essentially eliminated. Revascularization — the growth of new blood vessels toward the implanted follicles — begins within days and continues developing over the following weeks and months.
This biological window — from implantation through day fourteen — is when the aftercare requirements are most stringent, the consequences of non-compliance are most severe, and the decisions patients make about their behavior have the most direct impact on how many of their transplanted follicles survive to produce permanent hair. What happens outside this window matters too, but nothing that happens after day fourteen affects outcomes as immediately or as irreversibly as decisions made within the first two weeks.
Not Washing Correctly: Graft Loss, Infection, and Scarring
The washing protocol after a hair transplant is detailed and specific — specific products, specific technique, specific timing — for reasons that are directly connected to biological outcomes. Deviating from it in either direction creates problems that are predictable and preventable.
Washing too aggressively — using normal shampooing technique, applying direct water pressure from a showerhead, or rubbing the scalp with a towel during the first two weeks — applies mechanical force to grafts that are still anchored only by fibrin. The most serious consequence is graft dislodgement: physically removing implanted follicles from their new location before they have integrated into surrounding tissue. A dislodged graft cannot be re-implanted and is permanently lost.
Graft dislodgement from aggressive early washing is one of the most common preventable causes of lower-than-expected graft survival. It doesn’t require particularly rough handling to occur — normal hair washing force is sufficient to dislodge grafts in the first week. Patients who “didn’t realize” the protocol was so specific, or who felt the gentleness required was excessive, sometimes wash more vigorously than intended and lose grafts as a result.
Not washing at all — the opposite error, driven by anxiety about disturbing grafts — creates a different set of problems. Keeping the scalp unwashed allows bacterial accumulation around the healing graft and extraction sites. This bacterial buildup increases the risk of folliculitis — inflammation of the hair follicles — and outright infection, both of which can compromise graft survival and produce more visible scarring than clean-healing wounds. The daily washing protocol from day three or four onward is protective rather than risky; avoiding it to “protect” the grafts paradoxically compromises them.
Not washing also prevents the natural progression of scab shedding. Scabs that accumulate and harden around graft sites, rather than being progressively loosened by daily gentle washing, create their own risk: eventual forcible removal of hardened scabs requires more force than gentle washing would have, and that force applied at a later stage can still dislodge or damage grafts and produce worse scarring than the gradual natural shedding the washing protocol supports.
Picking or Scratching Scabs: The Most Consequential Mistake
Among the specific behaviors that most reliably compromise hair transplant outcomes, manually picking or scratching scabs off the recipient area during the first two weeks is both the most common and the most consequential.
Scabs form around each implanted graft site as a normal part of the wound-healing response. They are protective, temporary, and designed to shed naturally over ten to fourteen days with gentle daily washing. Forcibly removing them before they are ready to shed naturally does several things that directly compromise the result.
A scab that is not ready to shed is still attached to the underlying healing tissue. Pulling it off takes graft-anchoring tissue with it. The graft beneath may survive — the follicle is below the surface and not in the scab itself — but it has been subjected to mechanical disruption at a stage when it is most vulnerable to exactly that disruption. Depending on timing and force, this can compromise graft survival directly, dislodge the graft entirely, or produce a healing pattern that results in more visible scarring at the graft site.
The itching that drives the impulse to scratch is real and sometimes intense — particularly from days three through seven as healing progresses. This itching should be managed through appropriate alternatives: gentle patting, cool compresses, antihistamines if prescribed. The discomfort of managing itching without scratching is real. The discomfort of a lower-density result from compromised graft survival is permanent.
Sun Exposure During Healing: Prolonged Redness and Hyperpigmentation
UV radiation on a healing scalp causes specific problems that are well-documented and entirely preventable. The instruction to avoid direct sun exposure during the first three months of recovery is not overcautious — it reflects genuine clinical consequences of UV exposure on healing tissue.
The most immediate consequence of UV exposure during the healing phase is prolonged redness. The recipient area’s redness after a hair transplant reflects the inflammatory response of the healing tissue. This inflammation normally resolves progressively over weeks to months. UV radiation on healing scalp maintains the inflammatory state that would otherwise be resolving — essentially resetting the inflammatory clock each time it occurs and extending the period of visible redness beyond what would have been necessary without sun exposure.
The more significant long-term consequence is hyperpigmentation — patches of darkened skin in the recipient or donor areas. UV radiation stimulates melanocytes in healing tissue differently from how it affects intact skin, producing uneven pigmentation responses that can be more pronounced and longer-lasting than in fully healed skin. Post-inflammatory hyperpigmentation from a hair transplant can persist for months and is significantly more likely and more severe when the healing scalp has been exposed to UV during the vulnerable early healing phase.
For patients with darker skin tones, the risk of significant hyperpigmentation from sun exposure during healing is substantially higher, and the duration of any pigmentation changes is longer. This makes sun protection particularly important for these patients — though it is relevant for all patients regardless of skin tone.
The protective measure is simple: cover the head when outdoors during the first three months. A loose hat that doesn’t compress the recipient area is sufficient. The consequence of not doing this — months of unnecessarily prolonged redness and the possibility of significant lasting pigmentation changes — is disproportionate to the inconvenience of the protection.
Physical Activity Too Soon: Why Exercise Timing Matters
The restriction on strenuous physical activity in the first two weeks of hair transplant recovery is one of the instructions patients are most likely to underestimate or prematurely abandon. It has direct biological consequences that are worth understanding specifically.
Strenuous exercise increases blood pressure and heart rate, which increases blood flow throughout the body including to the scalp. During the first week, when grafts are held only by fibrin and the extraction and implantation wounds are still fresh, increased blood flow to the scalp raises the risk of bleeding from these sites. Post-procedure bleeding in the recipient area can dislodge grafts or disturb the healing process in ways that compromise graft survival and produce worse scarring. Bleeding from donor extraction sites, while less consequential for graft survival, complicates healing and increases infection risk.
Sweating during the first two weeks creates its own problems. Sweat is salty and slightly acidic, and in the recipient area it can irritate healing graft sites and increase bacterial accumulation in the same way that not washing does — but less controllably, because sweat exposure isn’t limited to specific application events. Patients who return to intense gym workouts in the first week are sweating heavily across an area of their scalp that is trying to heal from hundreds of small wounds simultaneously.
Bending forward significantly or performing activities that increase intracranial pressure — heavy weight lifting being the most common example — can increase blood flow to the scalp in ways that produce or worsen the forehead swelling that normally peaks around days two to four. This swelling is temporary and cosmetically uncomfortable rather than clinically dangerous, but unnecessarily prolonging or intensifying it is avoidable.
The standard recommendation is to avoid strenuous activity for the first two weeks and return to light exercise gradually from the third week, with full intensity exercise typically appropriate from weeks four to six. Patients who return to heavy training at one week because they “feel fine” are taking risks with their graft survival that the subjective feeling of physical readiness doesn’t reflect.
Alcohol in the Recovery Period: Multiple Mechanisms of Harm
The instruction to avoid alcohol — strictly for the first two weeks, and minimally for the first six months — reflects alcohol’s interference with multiple aspects of the recovery process simultaneously. This is not a generic health advisory; it is specific to how alcohol’s pharmacological effects interact with the biological requirements of hair transplant recovery.
Alcohol is a vasodilator — it widens blood vessels throughout the body. In the context of a recently performed hair transplant, this vasodilation increases blood flow to the scalp in ways that raise the risk of bleeding from extraction and implantation sites during the first week. The same mechanism that makes alcohol consumption ill-advised before the procedure because of surgical bleeding risk applies in the immediate post-procedure period.
Alcohol inhibits protein synthesis, which directly compromises the availability of amino acids for the cellular repair processes that healing tissue requires. The production of keratin — the structural protein that forms hair shafts — requires adequate amino acid availability. The tissue repair of both the donor extraction sites and the recipient implantation sites requires protein synthesis. Alcohol’s inhibition of these processes during the critical healing period is a genuine impediment to the quality of healing.
Alcohol depletes B vitamins — particularly folate and B12 — that are important for the cellular division occurring in recovering tissue. And it impairs sleep quality at a stage when sleep is one of the primary recovery tools available. A patient who drinks heavily in the first week of recovery is simultaneously increasing bleeding risk, impairing tissue repair, depleting micronutrients important for healing, and degrading sleep quality — all of which work against the biological processes the recovery depends on.
Beyond the first two weeks, the recommendation to minimize alcohol across the full six-month recovery and regrowth period reflects the cumulative impact of alcohol’s interference with protein synthesis and B vitamin status on the quality of the anagen re-entry phase — the period when transplanted follicles exit telogen and begin producing new permanent hair. This is a less acute effect than the first-week bleeding risk, but it is real and cumulative across months of continued exposure.
Sleeping Position: Why Head Elevation Matters
The instruction to sleep with the head elevated at approximately a 45-degree angle for the first three to five nights is one of the aftercare requirements patients most commonly rationalize away — it’s uncomfortable, it disrupts normal sleep, and its connection to the surgical result feels less obvious than instructions about washing or activity restriction. But its effects on the early recovery experience are specific and meaningful.
Lying flat increases blood flow to the scalp, which during the first days of recovery can increase swelling in the recipient area and particularly in the forehead, where anesthetic fluid migrates under gravity. The forehead and periorbital swelling that commonly develops on days two through four is primarily driven by this fluid migration, and head elevation during sleep directly reduces the gravitational pressure that drives it. Patients who sleep flat from the first night consistently develop more pronounced and longer-lasting swelling than those who maintain the recommended elevation.
Beyond the swelling consequence, lying flat during the first few days increases blood pressure in the scalp vessels relative to the elevated position, which can increase the risk of minor bleeding from donor and recipient sites in patients who move during sleep. This is a less directly consequential risk than aggressive washing, but it is an avoidable one.
The discomfort of sleeping elevated for a few nights is real. The forehead swelling that develops when patients don’t maintain it — sometimes significant enough to cause periorbital swelling that temporarily affects vision — is considerably more discomforting and longer-lasting. The trade-off clearly favors the temporary inconvenience of the pillow arrangement.
Smoking: The Most Underestimated Recovery Risk
Nicotine’s effects on the healing process are among the most well-established in surgical medicine, and they are directly relevant to hair transplant recovery in ways that are not always communicated with appropriate emphasis.
Nicotine is a potent vasoconstrictor — it narrows blood vessels and reduces blood flow to peripheral tissue including the scalp. During the critical period of graft revascularization — the process by which new blood vessels grow toward implanted follicles to re-establish their blood supply — reduced scalp blood flow creates a less favorable environment for this vascular ingrowth. Grafts in a poorly perfused environment have lower survival rates than those in well-oxygenated, well-perfused tissue.
The effect of smoking on wound healing more broadly is well-documented: smokers consistently demonstrate slower wound closure, higher infection rates, and worse scar formation than non-smokers across a wide range of surgical procedures. The donor area extraction sites and recipient implantation sites that need to heal cleanly after a hair transplant are subject to the same impairment.
The recommendation to avoid smoking for at least two weeks before and two to four weeks after the procedure reflects the most critical window. Continuing to smoke throughout the recovery period — particularly through the first month when revascularization is most active — represents a meaningful, ongoing impairment to the graft survival and healing processes that determine the final density of the result.
Patients who smoke should discuss this honestly with their surgeon during consultation — not because smoking is an absolute contraindication, but because its effects on the result are real enough to warrant an honest accounting of the risk and a genuine plan for the recovery period.
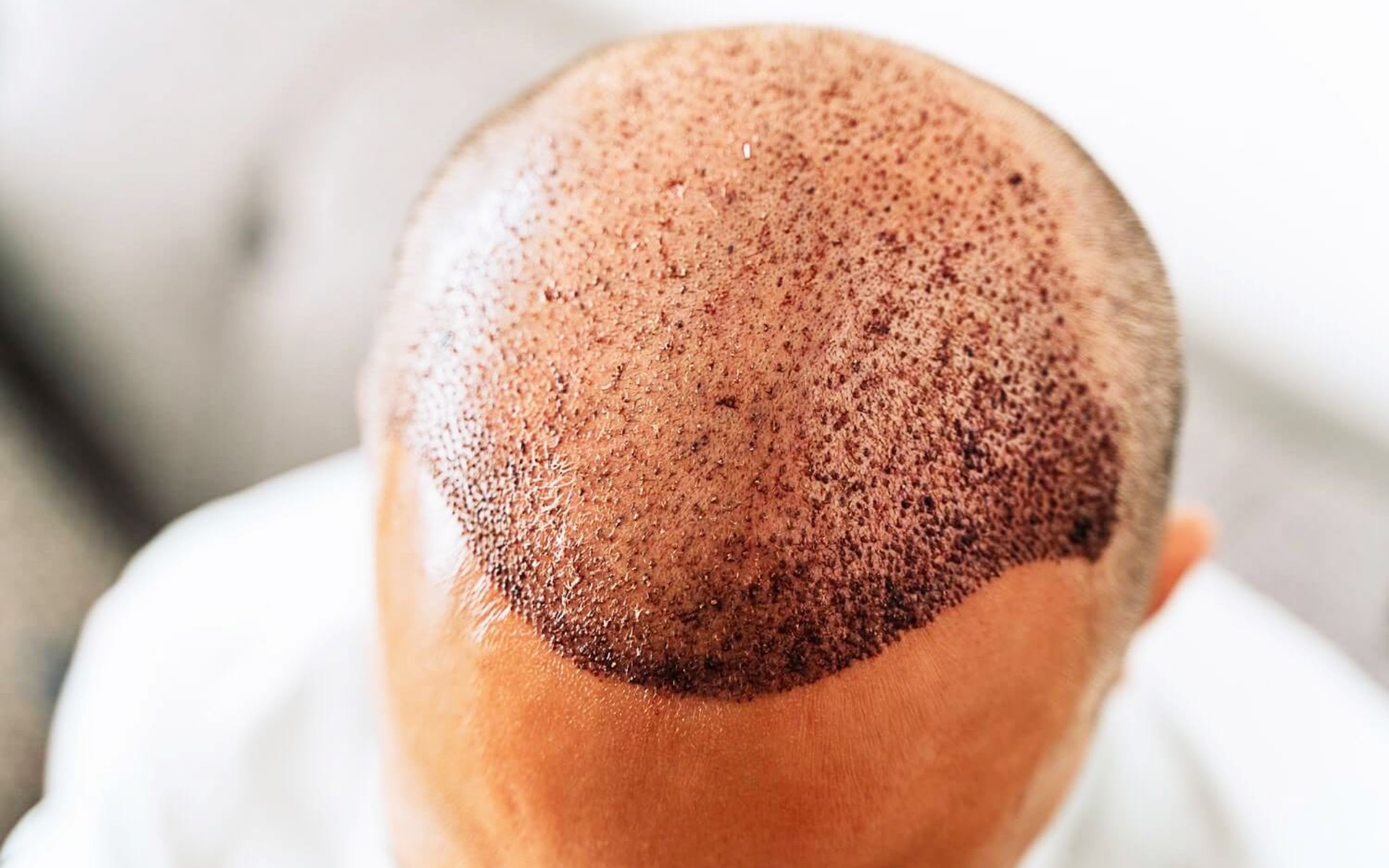
Wearing Tight Hats or Helmets Too Soon: Direct Graft Pressure
The instruction to avoid anything that compresses or puts direct pressure on the recipient area during the first two weeks is grounded in the same principle as the washing protocol: grafts held only by fibrin in the first week cannot withstand mechanical force without risk of dislodgement.
Tight hats, helmets, headbands, and any other headwear that sits directly on the recipient area create sustained compression against the healing graft sites. Unlike the brief mechanical force of water pressure or accidental contact, tight headwear maintains this pressure continuously — and sustained compression against fresh graft sites during the first week is a meaningful risk for both graft dislodgement and impaired blood supply to the healing tissue at those sites.
Loose hats — those that don’t compress the recipient area — are generally acceptable for sun protection from early in the recovery period. The distinction between loose protective headwear and tight compressive headwear is the clinically relevant one. Patients who wear fitted caps or helmets for work or sport within the first week are applying sustained compression to grafts that are still in their most vulnerable integration phase.
For patients who need head protection for work — particularly those who wear safety helmets — this requirement has practical implications that need to be planned around before the procedure. Returning to work that requires helmet use before the two-week point represents a genuine graft survival risk that may require adjusting the timing of the procedure or the return-to-work date.
Ignoring Warning Signs: When Delayed Response Creates Complications
The aftercare instructions for a hair transplant include guidance not only on what to do and avoid, but on when to contact the clinic — and this element of aftercare is sometimes the one patients are least attentive to.
Infection following a hair transplant is uncommon when proper aftercare is followed, but it does occur. The consequences of an untreated infection in the recipient area — progressive tissue damage, compromised graft survival in the affected zone, and worse scarring — are significantly more severe than the consequences of early-treated infection, which can typically be resolved with antibiotics with minimal impact on the overall result.
Patients who notice warning signs — increasing rather than decreasing redness or swelling after the first few days, discharge or unusual odor from donor or recipient sites, significant localized pain that worsens rather than improves, fever — and who delay contacting the clinic because they don’t want to “bother” anyone or assume the signs will resolve on their own, allow infections to progress that would have been easily managed if identified earlier.
The same principle applies to concerns about the healing process more broadly. Patients who notice what seems like unusual scabbing, unexpected bleeding after washing, or signs that something may have gone wrong with a graft site, and who don’t contact the clinic, sometimes discover weeks later that what they were seeing was an early indication of a problem that the clinic could have assessed and managed promptly.
The appropriate response to uncertainty during recovery is always to contact the clinic — not to self-diagnose and manage, not to research online and conclude that everything is probably fine, but to reach out to the people with the clinical knowledge to assess what the patient is describing. A brief conversation that resolves a concern early is always better than delayed presentation of a complication that has been given time to develop.
What Happens to the Result When Aftercare Is Poor
The cumulative effect of poor aftercare on the eventual hair transplant result can range from modest to significant depending on which instructions were not followed, how consistently they were not followed, and during which phase of recovery the failures occurred.
The most directly consequential failures are those that occur during the first two weeks and that involve mechanical force to the recipient area — aggressive washing, picking scabs, tight headwear, or strenuous activity — because these carry the risk of graft dislodgement and therefore permanent reduction in graft survival. A patient who loses ten percent of their grafts through poor early aftercare has permanently lost ten percent of the density that the procedure was designed to deliver. This is not recoverable — lost grafts cannot be replaced except through an additional procedure that draws from the same finite donor supply.
Failures in sun protection produce results that include unnecessarily prolonged redness and possible lasting hyperpigmentation — cosmetically significant though not affecting the fundamental density of the result. Failures in alcohol and smoking management produce impaired healing and potentially reduced graft survival through the mechanisms described above. Failures in nutritional management — not maintaining adequate protein, iron, vitamin D, and zinc status during the recovery period — can slow the anagen re-entry of transplanted follicles and produce a recovery that takes longer to show results than it should.
The resulting picture from consistently poor aftercare across multiple dimensions can be a result that falls meaningfully short of what the procedure was technically capable of producing: lower density than expected, more visible scarring in the donor or recipient areas, longer and more complicated healing, and in some cases complications like infection that require additional clinical intervention.
None of this is inevitable. All of it is preventable. The aftercare instructions exist precisely because the biological processes they support and the risks they mitigate are real — and following them is not optional additional effort beyond the procedure itself, but an integral part of the complete procedure whose outcome the patient is invested in.
At Hairpol, aftercare guidance is provided in comprehensive detail before the procedure so that patients understand not just what to do but why — because patients who understand the biological reasoning behind each instruction follow it more consistently than those following rules without context. The procedure is the beginning. The aftercare is how the result of that procedure is protected, optimized, and brought to its full potential.
The Bottom Line
Following aftercare instructions after a hair transplant is not supplementary to the procedure — it is part of the procedure. The surgical work creates the biological opportunity for permanent hair restoration. The aftercare in the weeks and months that follow is what determines whether that opportunity is fully realized.
The specific consequences of specific failures — graft loss from mechanical disruption, infection from inadequate hygiene, hyperpigmentation from sun exposure, impaired healing from smoking and alcohol — are predictable, documented, and preventable. Understanding them specifically rather than generally is what makes the difference between patients who protect their result through the recovery period and those who compromise it through well-intentioned but poorly informed decisions.
The investment in a hair transplant — of money, time, and the physical experience of the procedure and recovery — is significant. The aftercare that protects that investment costs nothing beyond attention, patience, and the temporary adjustments to routine that the first two to four weeks require. It is, by any measure, among the highest-return parts of the entire hair restoration process.
Frequently Asked Questions (FAQ)
What happens if you wash your hair too aggressively after a hair transplant?
Washing too aggressively after a hair transplant during the first two weeks carries the risk of graft dislodgement — physically removing implanted follicles from their new location before they have integrated into surrounding tissue. In the first days after the procedure, grafts are held in place only by a thin fibrin seal rather than by established tissue integration. Normal shampooing force — running fingers through hair, massaging shampoo in, rubbing with a towel — is sufficient to dislodge grafts anchored only by fibrin. A dislodged graft cannot be re-implanted and is permanently lost, directly reducing the density the procedure was designed to deliver. Aggressive washing also risks damaging the delicate scabs that protect healing graft sites, producing more visible scarring than naturally shed scabs would have. The correct washing protocol — gentle dabbing with a softening lotion, minimal-friction shampoo application, and lukewarm water flow rather than direct pressure — exists specifically to keep the scalp clean while protecting grafts through their critical integration window.
What happens if you pick scabs after a hair transplant?
Picking or scratching scabs off the recipient area during the first two weeks after a hair transplant is one of the most consequential aftercare mistakes and the one most likely to directly compromise the result. Scabs that are not ready to shed naturally are still attached to the underlying healing tissue. Forcibly removing them takes graft-anchoring tissue with them — potentially dislodging the grafts beneath or disrupting their integration at a stage when they are most vulnerable. Even when the graft itself survives, premature forcible scab removal leaves open wounds that heal with more visible scarring than naturally shed scabs would produce. The itching that drives the impulse to scratch is real and can be intense — particularly from days three to seven — but it should be managed through gentle patting, cool compresses, or prescribed antihistamines rather than scratching. Scabs left to shed naturally over ten to fourteen days through the gentle daily washing protocol produce the best healing outcomes. The temporary discomfort of not scratching is genuinely worth the permanent protection of the result.
What happens if you go in the sun too soon after a hair transplant?
UV exposure on a healing scalp after a hair transplant produces two specific consequences that are well-documented and entirely preventable. The most immediate is prolonged redness: the recipient area's post-procedural redness normally resolves progressively over weeks as the inflammatory response of healing tissue subsides. UV radiation on healing scalp maintains this inflammation rather than allowing it to resolve, effectively extending the period of visible redness beyond what would occur without sun exposure. The more significant long-term consequence is hyperpigmentation — patches of darkened skin in the recipient or donor areas. UV stimulates melanocytes in healing tissue differently from intact skin, producing uneven pigmentation responses that can persist for months. For patients with darker skin tones, the risk of significant hyperpigmentation and the duration of any pigmentation changes are substantially higher. Sun protection during the first three months — primarily through wearing a loose hat that doesn't compress the recipient area — is the simple and effective preventive measure. The consequences of neglecting it are disproportionate to the inconvenience of the protection.
Can exercise damage a hair transplant?
Strenuous exercise too soon after a hair transplant creates several specific risks that directly affect the surgical result. Increased blood pressure and heart rate from exercise raise blood flow to the scalp, increasing the risk of bleeding from donor extraction sites and recipient implantation sites during the first week when these wounds are still fresh. Bleeding in the recipient area can dislodge grafts or disrupt healing in ways that compromise graft survival and produce worse scarring. Heavy sweating creates bacterial accumulation across healing graft sites — similar to not washing, but less controllable — increasing infection risk. Activities involving significant bending or heavy weight lifting increase intracranial pressure and blood flow to the scalp in ways that worsen the forehead swelling that normally peaks around days two to four. The standard recommendation is to avoid strenuous activity for the first two weeks, return to light activity from week three, and resume full-intensity exercise from weeks four to six. Patients who return to heavy training at one week because they feel physically ready are taking risks with graft survival that the subjective feeling of readiness doesn't reflect.
What happens if you drink alcohol after a hair transplant?
Alcohol interferes with hair transplant recovery through multiple simultaneous mechanisms, which is why the instruction to avoid it — strictly for the first two weeks, minimally for the first six months — is clinically specific rather than a generic health advisory. As a vasodilator, alcohol widens blood vessels and increases scalp blood flow, raising the risk of bleeding from extraction and implantation sites during the first week. It inhibits protein synthesis, directly compromising the availability of amino acids for the tissue repair processes that healing wounds require — including the production of keratin for hair shaft growth. It depletes B vitamins — particularly folate and B12 — that support cellular division in recovering tissue. And it impairs sleep quality at a stage when sleep is one of the primary recovery tools available. Beyond the first two weeks, the cumulative impact of continued alcohol consumption on protein synthesis and B vitamin status during the anagen re-entry phase — when transplanted follicles exit telogen and begin producing new permanent hair — is a real and ongoing impairment to the recovery process. Heavy drinking in the first week of recovery simultaneously increases bleeding risk, impairs tissue repair, depletes healing-critical micronutrients, and degrades sleep.
Does smoking affect hair transplant results?
Yes — smoking has well-documented and specific negative effects on hair transplant outcomes through mechanisms that are directly relevant to graft survival and wound healing. Nicotine is a potent vasoconstrictor — it narrows blood vessels and reduces blood flow to peripheral tissue including the scalp. During the critical period of graft revascularization — when new blood vessels grow toward implanted follicles to re-establish their blood supply — reduced scalp blood flow creates a less favorable environment for this vascular ingrowth, directly compromising graft survival rates. Smokers also demonstrate consistently slower wound closure, higher infection rates, and worse scar formation than non-smokers across surgical procedures generally — effects that apply directly to the donor extraction sites and recipient implantation sites that need to heal cleanly. The recommendation to avoid smoking for at least two to four weeks around the procedure reflects the most critical window. Continuing to smoke throughout the recovery period — particularly through the first month when revascularization is most active — represents an ongoing, meaningful impairment to the biological processes that determine the final density of the result.
What happens if you wear a tight hat too soon after a hair transplant?
Wearing tight headwear — fitted caps, helmets, headbands — that compresses or puts direct pressure on the recipient area during the first two weeks after a hair transplant creates sustained mechanical force against healing graft sites. In the first week, when grafts are anchored only by a thin fibrin seal rather than established tissue integration, sustained compression is a meaningful risk for both graft dislodgement and impaired blood supply to the healing tissue at graft sites. Unlike the brief mechanical force of washing or accidental contact, tight headwear maintains this pressure continuously — which is why sustained compression is a more significant risk than brief contact of similar force. Loose headwear that doesn't compress the recipient area — such as a loose-fitting hat worn for sun protection — is generally acceptable. The distinction between loose protective headwear and tight compressive headwear is the clinically relevant one. Patients who need to wear safety helmets or other compressive headwear for work should plan the timing of their procedure and return-to-work date to ensure they are past the two-week critical window before resuming this headwear requirement.
What are the signs of infection after a hair transplant and what should I do?
Infection following a hair transplant is uncommon when proper aftercare is followed but does occur — and early identification and treatment produces dramatically better outcomes than delayed response. The warning signs that distinguish developing infection from normal recovery include: increasing rather than decreasing redness after the first few days, when the normal trajectory is progressive improvement; increasing warmth in a specific area of the donor or recipient zone beyond normal post-procedural heat; unusual discharge — particularly if colored or accompanied by unusual odor — from extraction or implantation sites; significant localized pain that worsens rather than improves after the first two to three days; and fever, which suggests a systemic inflammatory response. Any of these signs warrants immediate contact with the clinic rather than watchful waiting or self-management. Untreated infection can cause progressive tissue damage, compromised graft survival in the affected zone, and worse scarring — consequences that are significantly more severe than those of early-treated infection, which can typically be resolved with antibiotics with minimal impact on the overall result. When in doubt, contacting the clinic is always the right choice — no genuine concern about the healing process should be managed through uncertainty alone.