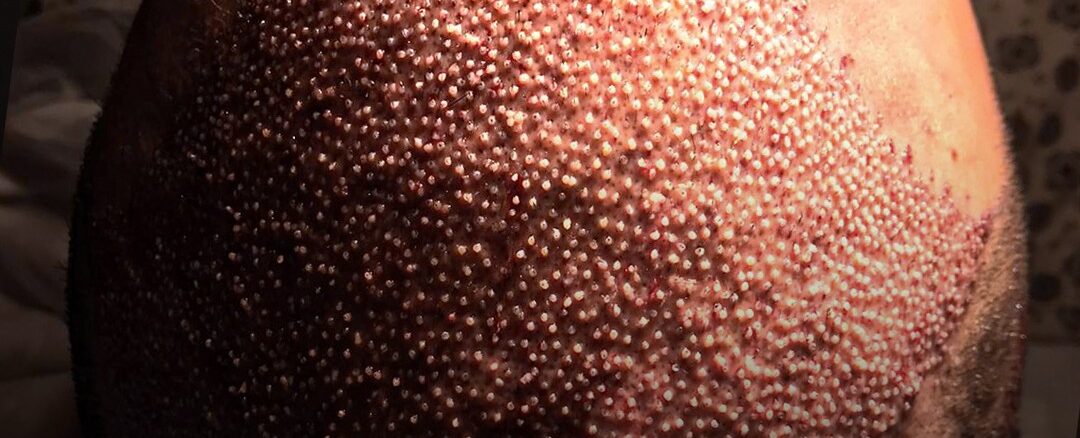
Ask most people what they picture when they think about a hair transplant, and they describe a hairline. A receding frontal hairline being restored, temples filled in, a natural-looking leading edge created where thinning had begun. This is the image that dominates before-and-after galleries, consultation materials, and the general public understanding of what the procedure does.
The crown tells a different story. Hair loss in the crown — the top-back area of the scalp where hair grows in a spiral or whorl pattern — is more common than many patients realize before it’s pointed out to them, and addressing it surgically involves a set of considerations that are genuinely distinct from frontal zone restoration. Not just technically different, but different in terms of how to plan, how to set expectations, how to evaluate results, and how to think about the decision to treat it at all.
Patients who go into a crown hair transplant expecting the same experience and the same result timeline as a frontal restoration are frequently surprised — sometimes pleasantly, more often not — by how differently the crown behaves. Understanding why the crown is different before committing to treating it is not a reason to avoid the decision. It’s the foundation for making the decision well.
The Anatomy of the Crown and Why It Complicates Everything
The frontal hairline has a clear logic. Hair grows in a relatively consistent direction — forward and slightly downward — and the line between hair and scalp, however it’s been shaped by loss or design, has a defined edge that creates a clear visual boundary. Restoration of the frontal zone is fundamentally about recreating that boundary and building density behind it.
The crown operates on completely different anatomical principles. Hair in the crown doesn’t grow in a single consistent direction. It radiates outward from a central point — the whorl — in a spiral pattern, with different sections of the crown growing in different directions depending on their position relative to that center. Hair directly ahead of the whorl grows forward. Hair to the right grows rightward. Hair behind the whorl grows backward. Hair to the left grows leftward. The entire area is organized around this central radiating pattern in a way that makes it one of the most directionally complex zones on the scalp.
This spiral organization means that implanting grafts in the crown without understanding and respecting each position’s specific growth direction produces hair that grows into conflict with itself. Grafts placed with incorrect angles relative to the whorl center will produce hair that crosses, fights against neighboring hairs, and sits wrong regardless of how long it grows or how it’s styled. A frontal hairline with slightly imperfect angles can often be forgiven by styling. The crown cannot be styled around fundamental directional errors — they’re three-dimensional and visible from multiple angles simultaneously.
The whorl itself adds another layer of complexity. In a person without hair loss, the whorl is a natural center of lower density where the radiating hair directions create a small zone where less hair covers the scalp surface. This is anatomically normal and present in everyone. In a hair transplant, recreating the whorl means intentionally designing a zone of slightly lower density in the center of the spiral, which feels counterintuitive to patients who want maximum density everywhere. But a crown without a natural-looking whorl doesn’t move correctly and reads as transplanted even when individual graft placement is technically excellent.
Why Crown Hair Loss Is Harder to Assess Than Frontal Loss
The frontal hairline announces itself clearly. The moment it begins receding, the change is visible in every mirror, every photograph, every interaction where someone looks at your face. The decline is measured against a reference point — where the hairline used to be — that both the patient and others can perceive directly.
Crown hair loss is different in how it presents and how it’s perceived. The crown is not visible to the person experiencing the loss in normal daily life. You cannot see the top-back of your own head without specific effort. Crown thinning is often noticed by others before the patient themselves — pointed out by a partner, visible in a photograph taken from behind, or revealed by an overhead angle in a shop window or security camera reflection that the patient encounters unexpectedly.
This delayed self-awareness creates a specific challenge for evaluating the extent of crown loss at any given time. Patients often come to consultations either significantly underestimating their crown loss — because they rarely see it directly — or significantly overestimating it, because the shock of a poorly angled photograph makes the thinning look more dramatic than it actually is under normal conditions.
Direct overhead lighting, which is the viewing angle most unfavorable to crown density, makes crown thinning look significantly worse than it does under neutral lighting at eye level. Most people interact with the world at eye level. But most patients evaluating their crown loss do so by holding a mirror over their head and looking at their crown under bathroom lighting, which is one of the worst possible assessment conditions available.
A proper clinical assessment of crown loss includes evaluating the area under consistent, neutral lighting at a standardized angle, measuring the extent of the thinning zone with calibrated reference points, and differentiating between what the crown looks like under extreme conditions versus how it appears in the normal social interactions it will be seen in most often. The difference between these assessments is significant and directly affects whether a crown hair transplant is appropriately indicated or whether the patient’s loss at this stage is better managed conservatively.
The Progression Problem: Why Timing Crown Treatment Is Different
Crown hair loss has a characteristic that frontal hair loss shares but that is more clinically significant in the crown context: it tends to be progressive in a way that is difficult to predict at any given moment.
Androgenetic hair loss — the genetic pattern loss that drives the vast majority of cases requiring hair transplant — follows a progression across the scalp that typically moves from the frontal zone backward toward the crown, while also expanding outward from the crown itself. The crown often represents the deepest point of loss in an ongoing pattern rather than a stable, defined zone of permanent baldness.
This progression creates a planning challenge that is more acute for the crown than for the frontal zone. A frontal hairline, once restored, sits at an anatomical boundary that doesn’t move dramatically even if surrounding hair continues to thin. The hairline can look increasingly isolated from mid-scalp density as hair loss progresses, but the hairline itself doesn’t expand.
The crown thinning zone, by contrast, expands outward as loss progresses. A patient who treats a modest crown thinning zone today may find that the treated area grows significantly over the following years, with the transplanted density island surrounded by increasingly thinned or absent native hair. The result can look like a patch of density surrounded by thinning — more obvious in some respects than the original loss because the contrast between transplanted and native hair is visible at the edge of the treated zone.
This is why crown hair transplant planning requires an explicit conversation about likely progression. Using grafts to treat the current crown extent without accounting for where the loss is heading is planning for today’s scalp, not the scalp the patient will have in ten years. The most experienced surgeons approach crown cases with a conservative initial treatment designed to account for likely expansion, preserving donor grafts for subsequent sessions that address the expanding periphery as progression continues.
The Donor Supply Calculation Is Different for Crown Cases
Every hair transplant draws from the same finite donor resource. The back and sides of the scalp contain follicles resistant to androgenetic loss, and the total number of viable grafts available to any individual is fixed by genetics, scalp laxity, donor density, and follicle characteristics. This donor supply needs to last across every procedure the patient will ever need.
The crown is notably graft-hungry. The area involved in even moderate crown thinning is larger than it appears when assessed from above, and achieving adequate density across a radiating spiral pattern requires substantial graft allocation. A crown thinning zone that looks modest from above may measure 80 to 120 square centimeters when properly mapped, and covering that area at adequate density requires 2,000 to 3,500 grafts depending on hair characteristics.
This creates a specific tension in cases where patients have both frontal and crown loss. The frontal zone is typically prioritized in planning because it has higher visual impact per graft — the hairline is what frames the face and is what the patient and others see most directly. Allocating a large portion of available donor grafts to the crown in a patient who also needs frontal restoration can compromise the frontal result or leave insufficient supply for future frontal sessions.
The reverse problem also exists. A patient who has received comprehensive frontal restoration using a significant portion of their lifetime donor supply may arrive at a crown treatment decision with limited remaining grafts. The crown requires more grafts than the remaining supply can provide for full coverage, and the planning must account for achieving the best possible partial result rather than comprehensive coverage.
The lifetime donor calculation is more consequential in crown cases and deserves explicit discussion in any consultation that addresses the crown.
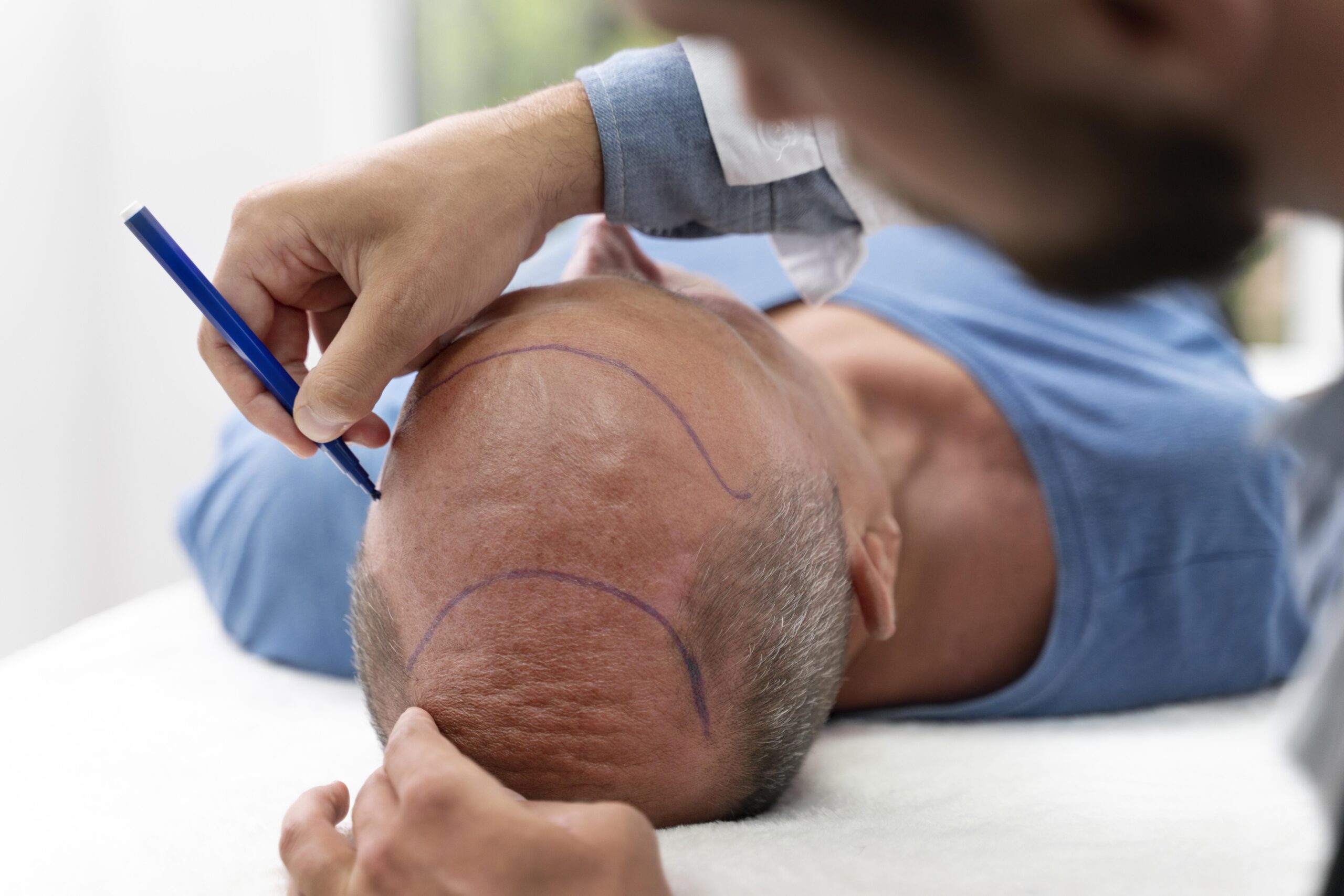
How Crown Results Are Perceived Differently From Frontal Results
A successful frontal hair transplant tends to produce results that are clear, visible, and immediately appreciated by both the patient and others. The hairline is restored. The temples are filled. The face looks different in a way that reads as more youthful and confident. The transformation is visible in photographs, in mirrors, in daily social interaction.
Crown results are perceived differently for several reasons that have nothing to do with the quality of the surgical outcome.
The viewing angle of the crown means that the patient themselves rarely sees the result directly. They may feel the difference — running a hand over a scalp that has density where there was thinning — but they can’t see it in the bathroom mirror during morning routine. Seeing the crown result requires specific effort: a second mirror, an overhead photograph, or asking someone to look from above. The result is real but not part of the patient’s daily visual experience of themselves in the way a restored hairline is.
Others see the crown result primarily from behind or above. The social feedback loop that reinforces satisfaction with a frontal result — noticing the hairline in every mirror, receiving compliments on looking well — is less active for a crown result, which can make the outcome feel less impactful even when objectively successful.
The expectation calibration for crown results needs to be different from frontal expectations as a result. A patient going into crown treatment expecting the same visceral satisfaction of seeing a restored hairline every morning is likely to feel underwhelmed, not because the procedure failed, but because the viewing geometry of the crown simply doesn’t deliver results in the same daily, self-visible way.
The Timeline Differences That Patients Need to Understand
The hair transplant timeline for the crown is consistently longer than for the frontal zone, and this is one of the most commonly underappreciated aspects of crown treatment.
The crown has a different blood supply pattern than the frontal scalp — the vascular network in the crown is somewhat less dense than in the frontal zone, which means revascularization of implanted grafts takes slightly longer. New blood vessels grow toward implanted follicles more slowly in the crown than in the front, and this affects the pace at which grafts transition from the implanted-but-resting state to the active-growing state.
The spiral growth pattern of the crown also means that early growth is less visually impactful than in the frontal zone. Individual hairs growing from the crown radiate outward and partially cancel each other’s coverage effect until they reach sufficient length to overlap and create the layering that produces visible density. Crown hairs, growing in multiple directions simultaneously, take longer to produce the overlapping coverage that reads as density.
Patients can expect to see meaningful crown growth appearing between months four and six, which is similar to the frontal timeline. But the improvement curve continues longer. Frontal results are often substantially complete by months nine to twelve. Crown results frequently continue developing through month twelve to eighteen, and in some patients the full result isn’t clearly established until the eighteen-month mark. Evaluating a crown result at six months and drawing conclusions about the final outcome is premature in a way that it isn’t quite for frontal results assessed at the same point.
The Lighting Problem and Why Crown Patients Must Understand It
The crown is the zone of the scalp most affected by lighting conditions, and this creates a specific psychological challenge for patients during recovery and even after full results are achieved.
Overhead lighting — the most common indoor lighting in offices, shops, restaurants, and bathrooms — shines directly down onto the crown. This downward angle maximizes scalp reflection between hair shafts and minimizes the shadowing that longer hair creates when light comes from the side or at an angle. The result is that the crown consistently appears thinner under overhead lighting than it does under other lighting conditions, regardless of the actual density achieved.
This is true for everyone, not just for patients who have had hair transplants. People with naturally thick crown hair look thinner under overhead lighting than under side-lit or natural outdoor conditions. But for patients who have received a crown hair transplant and are evaluating their result, the consistent appearance of thinness under overhead lighting creates a distorted picture of what the actual outcome is.
Patients who assess their crown result primarily by looking in a bathroom mirror under overhead lighting will consistently underestimate how good their result is. Understanding this lighting dynamic before the procedure helps patients interpret what they see during recovery more accurately and reduces the psychological difficulty of the months when the result is still developing.
The practical guidance is to assess crown results under natural outdoor lighting, at eye level if possible using a mirror, and to avoid treating overhead bathroom lighting as the reference condition. Photographs taken outdoors in diffused natural light give a significantly more accurate picture of crown density than those taken under indoor overhead lighting.
Conservative Planning: The Correct Approach to Crown Treatment
Given the combination of factors that make crown hair transplants more complex than frontal procedures, the appropriate surgical approach is more conservative than many patients initially want to hear.
A conservative crown treatment means starting with enough grafts to create meaningful density improvement across the central thinning zone, while deliberately not chasing the full extent of current loss. It means designing the transplanted area with outward-expanding loss in mind, creating a central density zone that will still look natural and intentional as the surrounding loss progresses. It means reserving donor grafts for future sessions that address the expanding periphery rather than exhausting supply attempting to cover everything in one procedure.
The patient’s natural instinct in a consultation is often to ask for maximum coverage of the currently visible thinning. The surgeon’s responsibility is to explain why maximum coverage today is not always the same as the best long-term outcome. A densely packed central crown result surrounded by untreated, progressively thinning native hair will look less natural in five years than a more modestly treated central zone that allows for logical future expansion.
When Crown Treatment Makes Sense and When It Doesn’t
Not every patient with crown thinning is a good candidate for surgical treatment, and responsible consultation includes an honest assessment of whether the timing and the patient’s specific situation support proceeding.
Crown treatment makes most sense when the thinning has been stable for a meaningful period — ideally one to two years — indicating that the current extent of loss is not rapidly expanding and can be planned around with more confidence. It makes sense when the patient has adequate donor supply available after any frontal requirements have been accounted for. It makes sense when the patient has appropriate expectations about timeline, visibility of results, and the likelihood of future sessions as progression continues.
Medical management — finasteride, minoxidil, or both — should be considered before or alongside crown surgical treatment, because these medications can slow or partially reverse crown thinning in patients who respond well. A patient who begins finasteride and experiences significant crown improvement over six to twelve months may find that the surgical treatment they were planning is no longer indicated, or can be delayed significantly.
Crown treatment is more appropriately delayed when the loss is clearly still progressing rapidly, when the patient has limited remaining donor supply after prior procedures, when the patient is young enough that the long-term trajectory of loss remains highly uncertain, or when the patient’s expectations about results don’t align with what crown surgery can realistically deliver.
What the Result Actually Looks Like
When crown treatment is planned well, executed with attention to directional complexity and whorl design, and given the time it needs to fully mature, the result is a genuinely natural-looking improvement in crown density that holds up under varied viewing conditions and ages appropriately as the patient’s hair and face continue to develop.
It won’t look like a person who never lost hair in the crown. The density achievable through transplantation is lower than native density, and the crown’s light sensitivity means there will always be viewing conditions — directly overhead, under harsh lighting — where the treated area looks thinner than ideal. These are realities of crown restoration that honest planning acknowledges rather than oversells.
What it will look like is a crown that has coverage where there was significant thinning, that moves and flows naturally because the directional design was respected, that doesn’t announce itself as transplanted because the whorl was properly reconstructed and the angles were correct, and that continues to look appropriate as the patient ages because the planning accounted for ongoing loss rather than only today’s snapshot.
That outcome is achievable with the right surgical team, the right patient selection, and the right expectations going in. It just requires understanding, before anything else, that the crown is not the frontal zone, and the approach that works brilliantly for one will produce frustrating results when applied without modification to the other.
Frequently Asked Questions (FAQ)
Why is a hair transplant for the crown different from a frontal hair transplant?
A crown hair transplant differs from frontal zone restoration in several fundamental ways. The crown's anatomy is based on a spiral or whorl growth pattern where hair radiates outward in multiple directions from a central point — making directional implantation significantly more complex than the relatively consistent forward direction of frontal hair. Crown hair loss is harder to self-assess accurately because the crown isn't visible in normal daily life, and patients frequently misestimate their extent of loss. The crown is more light-sensitive than the frontal zone, consistently appearing thinner under overhead lighting regardless of actual density. The hair transplant timeline for crown results extends longer — often through month eighteen — and results are perceived differently because they're less self-visible in daily mirrors than a restored hairline.
How many grafts are needed for a crown hair transplant?
The crown is notably graft-hungry relative to its visual appearance from above. A crown thinning zone that looks modest in a mirror may measure 80 to 120 square centimeters when properly mapped — and covering that area at adequate density typically requires 2,000 to 3,500 grafts depending on individual hair characteristics including caliber, color contrast, and curl pattern. This substantial graft requirement creates important planning tensions for patients who also have frontal loss, since the frontal zone is typically prioritized for its higher visual impact per graft. A responsible hair transplant plan for crown cases accounts for the lifetime donor supply across all likely future procedures, not only the grafts needed for the current session.
Why does crown hair loss look worse under bathroom lighting?
The crown is the zone of the scalp most affected by lighting conditions because overhead lighting — the most common type in bathrooms, offices, and restaurants — shines directly downward onto it. This angle maximizes scalp reflection between hair shafts and minimizes the shadowing effect that longer hair creates when light comes from the side. The result is that the crown consistently appears thinner under overhead lighting than under any other conditions, regardless of actual density. This applies to everyone — even people with naturally dense crown hair appear thinner under overhead lighting. Patients evaluating their crown hair transplant result under bathroom lighting will consistently underestimate their outcome. The accurate way to assess crown density is under natural outdoor diffused lighting or side-lit conditions, not directly overhead indoor lighting.
How long does it take to see results after a crown hair transplant?
The hair transplant timeline for the crown is consistently longer than for the frontal zone. Meaningful crown growth typically begins appearing between months four and six, similar to the frontal timeline for initial emergence. However, the improvement curve continues significantly longer — frontal results are often substantially complete by months nine to twelve, while crown results frequently continue developing through month twelve to eighteen. In some patients, the full crown result isn't clearly established until the eighteen-month mark. This extended timeline reflects the crown's less dense vascular network — which means revascularization of implanted grafts takes longer — and the spiral growth pattern, where hairs growing in multiple directions take more time to create visible overlapping coverage than hairs all growing in the same forward direction.
Why does the crown require conservative planning in hair transplant surgery?
Conservative planning for crown hair transplants is essential because crown hair loss tends to be progressive in a way that is more clinically significant than frontal loss. The frontal hairline, once restored, sits at a relatively stable anatomical boundary even as surrounding hair continues to thin. The crown thinning zone, by contrast, expands outward as androgenetic hair loss progresses — meaning a patient who treats their full current crown extent may find the treated zone surrounded by expanding untreated thinning within a few years. This produces a result that looks like a patch of density surrounded by loss, which can be more conspicuous than the original thinning. Conservative planning means treating the central zone while reserving donor grafts for future sessions that address the expanding periphery — prioritizing the ten-year result over the six-month result.
Should I treat my crown or frontal zone first in a hair transplant?
When both frontal and crown hair loss are present, the frontal zone is typically prioritized in hair transplant planning because it delivers higher visual impact per graft — the hairline frames the face and is what both the patient and others see most directly in daily interaction. Crown results, while meaningful, are less self-visible and perceived primarily by others viewing from behind or above. Allocating a large portion of available donor grafts to the crown in a patient who also needs frontal restoration risks compromising the frontal result or depleting supply for future frontal sessions. That said, the correct sequencing depends on individual factors including the extent of loss in each zone, the patient's total donor supply, and whether the crown loss is in an active progression phase — all of which should be addressed explicitly in consultation.
When is a crown hair transplant not recommended?
Crown treatment is more appropriately delayed or declined in several specific situations. When crown hair loss is clearly still progressing rapidly, treating the current extent creates a moving target that the donor supply may not be able to keep pace with as the thinning zone expands. When a patient has limited remaining donor supply from prior procedures, the crown's substantial graft requirements may exceed what's available for meaningful coverage. When a patient is young enough that the long-term trajectory of loss is still highly uncertain, committing significant donor grafts to the crown risks depleting supply before the full scope of lifetime loss is understood. Medical management with finasteride or minoxidil should be tried first — a patient who responds significantly may find surgical intervention no longer indicated or may be able to defer it with a much clearer picture of their pattern.
What does a successful crown hair transplant actually look like?
A well-executed crown hair transplant, planned conservatively and given time to fully mature, produces a crown that has coverage where there was significant thinning, moves and flows naturally because the whorl design and directional angles were respected, and doesn't announce itself as transplanted to others viewing from above. It will not look identical to a crown that never experienced hair loss — the density achievable through transplantation is lower than native density, and the crown's inherent light sensitivity means overhead lighting will always reveal some scalp visibility. These are honest realities of hair transplant crown restoration. What it does deliver is meaningful, natural-looking coverage that continues to look appropriate as the patient ages — provided the planning accounted for ongoing progression rather than treating only the snapshot of loss visible at the time of the procedure. Crown results typically require evaluation at twelve to eighteen months rather than six to nine to reflect the full outcome.